The Sword Summary Warm-up
Don’t have time for the full workout? Here’s the quick version.
- Lower back pain at night often comes down to position, support, and long stretches of stillness, not automatically to something serious.¹
- A few practical changes, like adjusting how you sleep or using pillows more strategically, can reduce pressure on your lower back.
- If the pain keeps interrupting sleep or starts shaping your day, physical therapy can help you address what is driving it.²
Why lower back pain feels worse at night
Lower back pain often feels more intense at night because your body loses the constant motion that helps spread load around. During the day, you shift without thinking. You bend to pick something up, lean in a chair, change direction mid-step. Overnight, all of that movement disappears. The same joints, muscles, and soft tissues hold the same position for hours.
That is why a back that feels manageable at 3pm can feel stiff, sore, or strangely sharp at 3am. Sleep does not create the problem out of nowhere. It simply gives pressure and irritation more time to settle in.
There is another layer to it, too. Pain and poor sleep tend to keep each other company. Research suggests sleep may influence both pain intensity and recovery in low back pain, while chronic pain more broadly is known to disrupt sleep and heighten pain sensitivity.³ ⁴ A rough night can leave you more sensitive the next day, and a tense, overloaded back can make the next night harder again.
How sleep position affects your lower back

Your spine usually feels best when its natural curves are supported, not flattened and not pushed into an exaggerated arch. Some positions let your body settle. Others leave you waking up like you spent the night bracing.
- If you sleep on your back without support under your knees, your lower back may flatten more than it likes.
- If you sleep on your stomach, your lower back often falls into more extension while your neck twists off to one side. Hours of that can leave your back feeling irritated before the day has even started.
- Side sleeping often feels better, but even that depends on what the rest of your body is doing. When the top leg drops forward without support, the pelvis rotates and the lower back follows.
What feels soft and comfortable in the moment can leave your spine doing quiet extra work all night.
Best sleeping positions for lower back pain
You don't need to find a perfect or magical position. Instead, it's best to focus on giving your back more space and less pressure. Here are three options you can try that should all help to reduce lower back pain at night and allow your back to rest in a more natural position.
- Back sleeping with knee support: A pillow under your knees can soften the pull through the lower back and help distribute pressure more evenly. For many people, it takes the edge off that first-morning stiffness.
- Side sleeping with a pillow between knees: This setup often helps keep the pelvis steadier and reduces twisting through the lower spine. It is one of the simplest changes people notice quickly.
- If you shift positions overnight: Most people move in their sleep. That is not a problem to solve. What helps is setting things up so that when you do shift, your back is not paying for it by morning.

Small changes that can help reduce nighttime back pain
You do not need to rebuild your whole bedroom to test what helps. In fact, changing too much at once usually makes it harder to tell what is working.
Start with the pieces closest to your body. Pillow height is one of them. If your neck is tipped too far up or down, your spine often feels the ripple effect by morning. Support under or between your legs is another. These changes are simple, but sometimes they are the difference between waking up guarded and waking up able to move.
Mattresses matter, just not always in the dramatic way people expect. A sagging mattress can absolutely add strain. Still, even an expensive replacement will not solve the problem if your positioning or movement habits are doing part of the work.
Try these changes for a week
- Add a pillow under your knees if you sleep on your back.
- Place a pillow between your knees if you sleep on your side.
- Avoid stomach sleeping if mornings are consistently worse after it.
- Move gently before getting out of bed, especially if you wake up stiff.
Think of these as clues, not cures. When one of them helps, it tells you something useful about how your back wants to be supported.
Physical therapy can address the root cause of back pain
Low back pain is incredibly common. The World Health Organization identifies it as the leading cause of disability worldwide.⁶ The more useful question, then, is often not “Why does this hurt only at night?” but “What is my back reacting to at night and how do I prevent it?”
When position changes help only a little, the real issue often sits upstream. Your back may be carrying too much load during the day. Certain muscles may be gripping instead of supporting. You may be moving around pain in ways that make nighttime feel worse, even if the night itself is not the true source of the problem.
Physical therapy can help you diagnose the specific problem, manage the symptoms effectively, and work on a plan to prevent future flare ups. A physical therapist can look at how you move, where you are compensating, what seems overly sensitive, and which patterns are keeping your back working harder than it needs to. For many people, that is the moment the puzzle starts to make sense.
How Thrive AI physical therapy supports recovery from home
If your back pain keeps returning, you will likely benefits from physical therapy to help manage and prevent the pain. Traditional physical therapy requires you to travel to an in-clinic appointment during the day. Often, by this time, your symptoms are muted. You really need help in the moment when the pain and discomfort peaks. That is where Thrive’s personalized 24/7 care plans are so effective.
Sword Health’s Thrive is an AI physical therapy program that gives members access to a personalized care plan from the comfort of home. Thrive is accessible through the Sword app at any time or place, and it’s clinically proven to be effective in reducing pain for back, joint, and muscle pain.² ³
Members follow a custom plan designed by a Pain Specialist who holds a Doctor of Physical Therapy. All sessions are delivered with Vision AI guidance via the Sword app. Thrive gives audio and visual direction with real-time form correction from Phoenix, Sword’s AI Care Specialist.
Get started with Sword Thrive in 4 easy steps
1. Tell us about you
Share where you’re feeling pain, your medical history, and your lifestyle so we can tailor your care from the start.

2. Choose your clinician
Pick your dedicated physical therapist. They will guide your recovery and adjust your plan as you progress.

3. Start your personalized plan
Using the Sword app, open your personalized care plan and start your recovery. Phoenix, our AI Care Specialist, will guide your progress.
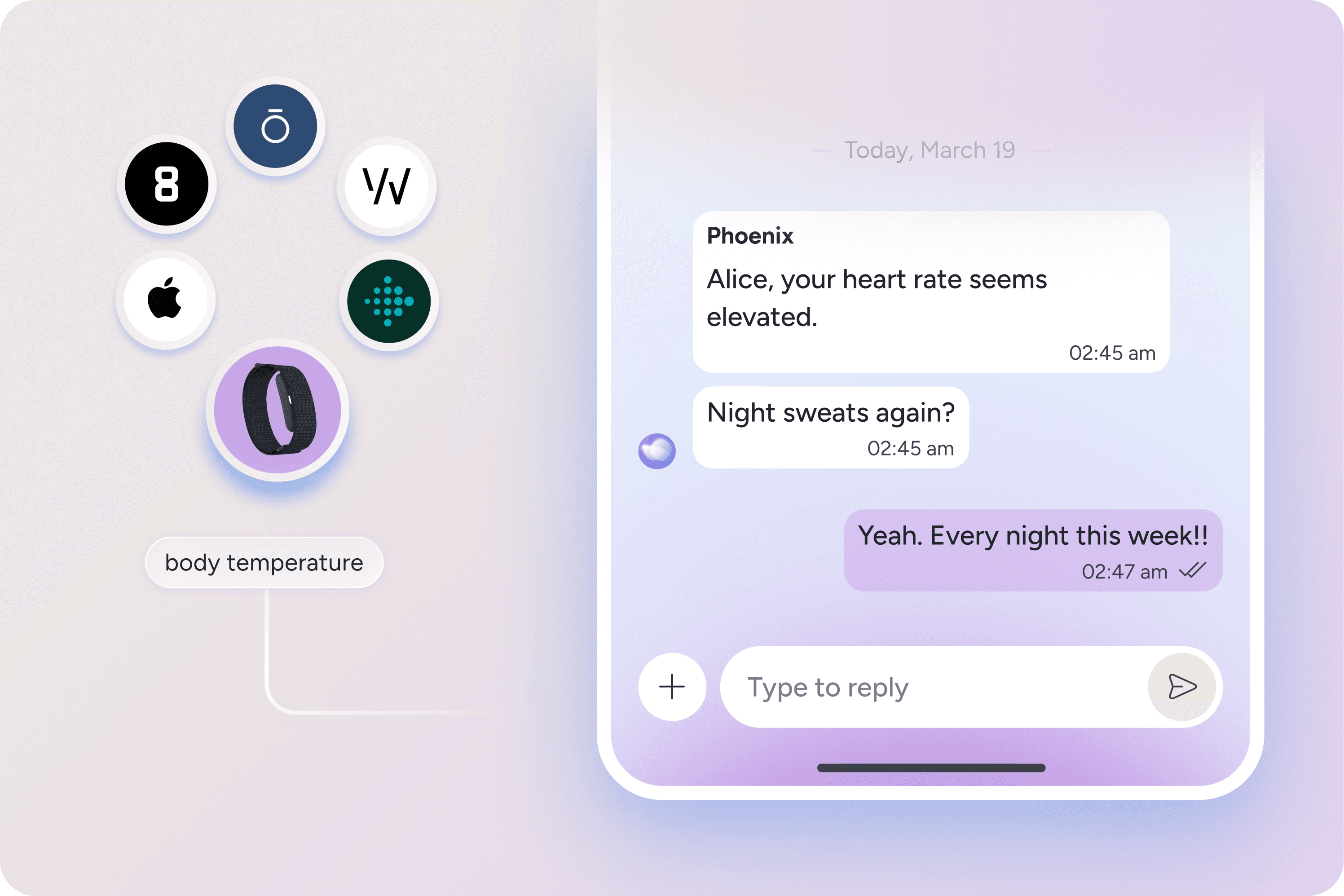
4. Connect your apps for smarter care
Thrive can use your wearable and calendar data to match your routines, key life events, and work patterns to proactively adjust your plan for even better results.
There is good evidence behind this approach. A study in people with chronic shoulder pain found that remote care helped people improve in function and symptoms at about the same rate, with no meaningful difference between the two groups.²
Care continues between check-ins, adapts based on your progress, and is available when you need it rather than only when you can schedule it. That structure is also why Thrive members complete their program at a rate of 81%.⁸ Half of the people who start traditional in-person physical therapy stop going after just four sessions. Not because the care does not work. Because the friction of getting there erodes their momentum.⁹
When care fits into your life, you finish it. Thrive user data shows that 69% of all Thrive members are free from limiting pain after completing their care programme⁷.

When nighttime back pain needs more attention
Some nighttime back pain fades once you get moving, but often this pain can develop and start to gradually take over more territory. It wakes you more often. It makes bedtime feel like trial and error. then it follows you into the morning and lingers longer than it used to.
That is usually the point where it is worth looking beyond sleep position alone. If the pain keeps waking you, if you still cannot get comfortable after trying simple adjustments, or if stiffness hangs around well into the day, a physical therapist can help sort out what is actually driving it.
It is also worth paying attention if the pain starts spreading into your hip, buttock, or leg, or if it changes character and feels sharper, more persistent, or more limiting. Those patterns do not automatically signal something serious, but they do suggest the story may be bigger than a sleep position problem.
Urgent in-person medical evaluation matters if red flag symptoms appear, such as bowel or bladder changes, progressive weakness, saddle numbness, significant trauma, fever, or severe unrelenting pain that does not ease with rest.⁵
Get back control of your nighttime back pain
Nighttime back pain has a way of shrinking life around it. People start planning for the bad mornings, moving more cautiously and stop trusting sleep. The cycle compounds as less sleep leads to more stress, tighter muscles, and often more pain.
The right support can interrupt that pattern. Not overnight, but by reducing the strain your back carries into the night in the first place. When that starts to happen, sleep feels less like a trigger and more like recovery again.
If you are not sure whether Thrive is included in your health insurance plan, the eligibility check is the fastest way to find out. Check if you're eligible through your employer benefits plan (it takes less than two minutes).

