The Sword Summary Warm-up
Don’t have time for the full workout? Here’s the quick version.
- Walking can trigger lower back pain for structural reasons. Your spine, muscles, or joints may be sending pain signals in response to repetitive motion or posture.
- Not all back pain during walking means you should stop moving. For most people, staying active with smart modifications is more helpful than prolonged rest.¹
- Patterns matter. When pain appears during your walk, how much walking you can do before it flares, and whether it settles with rest can help a physical therapist understand what may be driving it.
- What may help ranges from movement modification and pacing strategies to professional evaluation and a more personalized recovery plan.²
Why walking sometimes triggers lower back pain
You decide to take a walk. It’s something you’ve always done, something people tell you is good for your back. And yet, somewhere around the 10-minute mark, or after a certain distance, that dreaded lower back pain arrives. It builds in your lower back, sometimes sharp, sometimes aching. You slow down, then stop completely, knowing you will have to spend the rest of the day managing it.
Exercise is often recommended for low back pain, and for most people, staying active is more helpful than bed rest.¹ But walking is also repetitive and requires weight-bearing for an extended period. That can expose issues in posture, joint mobility, muscle coordination, or movement patterns that may not show up as clearly during other activities.
Your lower back is not a single structure. It is a system of vertebrae, discs, joints, muscles, ligaments, and nerves working together. When you walk, that system absorbs load, manages rotation, and responds to repeated impact. If one part of that system is not moving or supporting you well, symptoms can build over time.
That does not necessarily mean something serious is wrong and you may be able to manage and prevent future pain with the right approach.
The difference between movement that helps and movement that hurts
This is where the advice can seem mixed. You may have heard that movement is medicine, that staying active helps low back pain, and that complete rest can slow recovery. Broadly, that is consistent with clinical guidance.¹ ²
But not all movement feels the same, and not all movement is helpful in the same way at the same time. When your lower back starts sending pain signals during walking, your body may respond with guarding. That can show up as muscle tension, stiffness, and a sense that your back is bracing against the movement. In that situation, pushing harder through worsening pain is not always helpful. A better approach is often to stay active while changing the way you walk.
That may mean walking more slowly, going a shorter distance, choosing flatter surfaces, or taking breaks before symptoms build too far. For many people, that kind of modification is more effective than either stopping completely or trying to push through.¹ Some people improve with those changes alone. Others also need strengthening, mobility work, or a more targeted plan from a physical therapist.²
How to understand the patterns of your lower back pain
Your pain pattern can offer clues. Gather as much of these useful insights as you can and take some notes, either in your mobile phone or with a pad and pen. These details will really help a physical therapist make a more informed assessment.
- Pay attention to when the pain begins: Does it start right away, or only after a certain amount of time or distance? Does it show up on hills, uneven ground, or hard surfaces? Does it ease quickly when you stop, or linger for hours?
- Notice what the back pain feels like: Is it sharp and pinpointed, or more of a broad ache? Does it stay in your lower back, or travel into your buttock or leg? Does it ease as you warm up, or build the longer you go?
- Track your recovery: If a short walk leaves you sore for the rest of the day, that means something different from discomfort that settles within 20 to 30 minutes.
- Pay attention to your sleep and stress: Sleep and pain influence each other in both directions. In one published study of people with upper limb and spine conditions in a digital musculoskeletal care program, 78.0% of eligible patients reported sleep disturbance at baseline.³ If your sleep is off or your stress is high, your nervous system may be more reactive, and walking pain may feel harder to manage.
These details will also help you start to manage and reduce your symptoms more effectively, Read on to understand how you can start to use your own tactics to reduce your back pain while walking (and after movement if the symptoms start to flare).

Tips that might help reduce lower back pain when walking
If walking-related pain is relatively new or not too limiting yet, a few changes may help:
- Slow down and shorten your distance: For many people, reducing the dose of walking is the simplest place to start.
- Check your posture: A tall but relaxed posture, without slumping forward or leaning back excessively, may help reduce strain.
- Choose easier surfaces: Flat, even ground is often easier to tolerate than hills, trails, or uneven pavement.
- Consider your footwear: Shoes that are worn out or not supportive for you can change how force travels up the chain.
- Add targeted exercise if needed: Exercise is part of guideline-based care for low back pain, but the right mix depends on the person.²
Keep moving, just manage your walking and day-to-day movements differently. For most uncomplicated lower back pain, prolonged bed rest is not recommended, so you should not actively avoid movement. Staying as active as possible within your tolerance is usually the better path.¹

Physical therapy can address the root cause of lower back pain
Low back pain is incredibly common. The World Health Organization identifies it as the leading cause of disability worldwide.⁶ The more useful question, then, is often not “Why does my back pain flare up when I'm walking?” but “What is my back reacting and how do I prevent it?”
When the suggested changes and tactics above don't help to reduce the pain while walking, the real issue often sits upstream. Your back may be carrying too much load during the day. Certain muscles may be gripping instead of supporting. You may be moving around in awkward posture to compromise and avoid certain positions. Often, the avoidance of movement itself can contribute significantly to the pain as your back is consistently static in one position.
Physical therapy can help you diagnose the specific problem, manage the symptoms effectively, and work on a plan to prevent future flare ups. A physical therapist can look at how you move, where you are compensating, what seems overly sensitive, and which patterns are keeping your back working harder than it needs to. For many people, that is the moment the puzzle starts to make sense.
When walking pain is a reason to seek professional support
Not every episode of lower back pain during walking needs professional evaluation, but some situations do.
- If your pain is progressively worsening, limiting work or daily activities, or not improving after a few weeks of thoughtful modification, it is reasonable to get assessed.
- If pain radiates into your leg or foot, or comes with tingling or numbness, that can suggest nerve involvement and is worth evaluating.
- If symptoms started after a fall, a heavy lift, or another injury, an assessment can help rule out a more significant problem.
Some symptoms should be treated as red flags: New bowel or bladder dysfunction, saddle numbness, or progressive leg weakness need urgent medical evaluation.
For many cases of ongoing walking-related lower back pain, physical therapy is a practical first step. A physical therapist can assess your movement, identify likely drivers, and build a plan around your symptoms and goals.²
How Thrive's expert-guided pain care supports recovery from home
If your lower back pain keeps returning, this is a good sign that physical therapy can help you reduce and prevent the pain more effectively than if you just try to manage your symptoms yourself. A physical therapist does something simple but valuable. They look for the reason your pain is happening. That usually starts with listening to your history and then assessing how you walk, bend, rotate, and load your spine and hips. They may look at strength, flexibility, balance, and symptom response.
Traditional physical therapy requires you to travel to an in-clinic appointment during the day. For many people, it's hard to juggle work and family priorities to schedule in a session at these times, then commute to a busy clinic. You really need help in the moment when the pain and discomfort peaks. That is where Thrive’s personalized 24/7 care plans are so effective.
Sword Health’s Thrive is an AI physical therapy program that gives members access to a personalized care plan from the comfort of home. Thrive is accessible through the Sword app at any time or place, and it’s clinically proven to be effective in reducing pain for back, joint, and muscle pain.² ³
Members follow a custom plan designed by a Pain Specialist who holds a Doctor of Physical Therapy. All sessions are delivered with Vision AI guidance via the Sword app. Thrive gives audio and visual direction with real-time form correction from Phoenix, Sword’s AI Care Specialist.
Get started with Sword Thrive in 4 easy steps
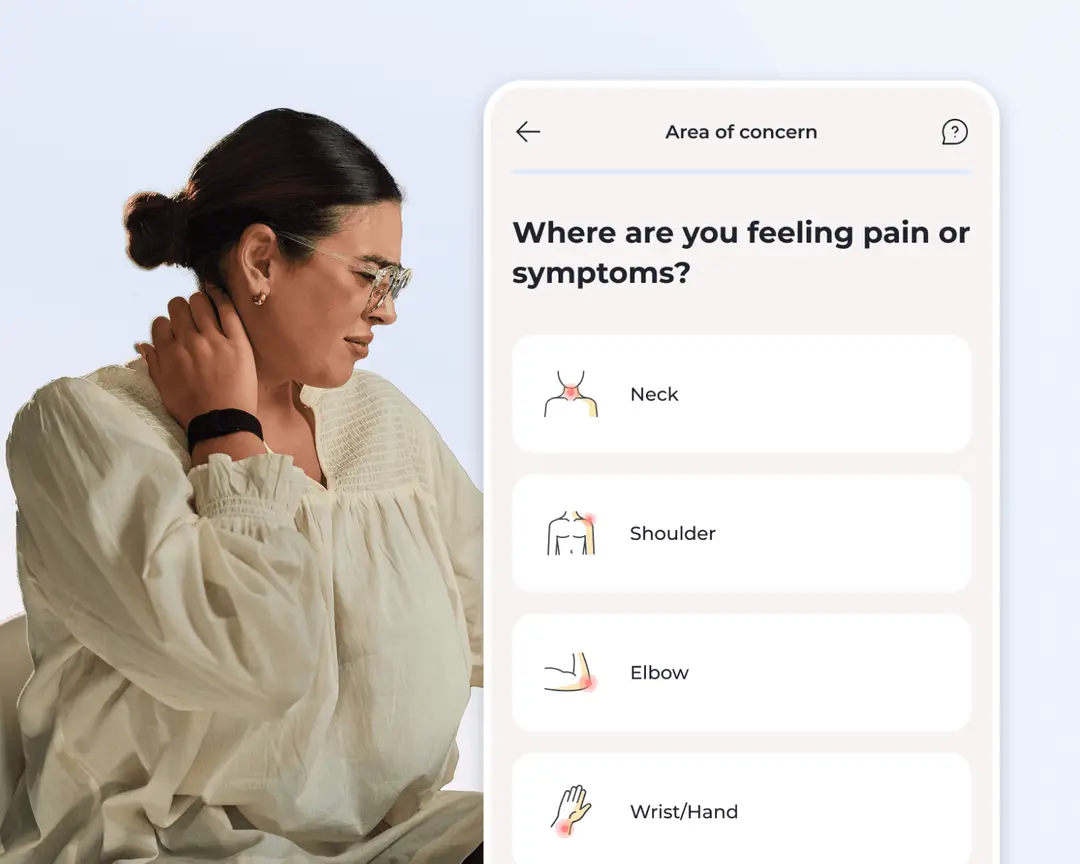
1. Tell us about you
Share where you’re feeling pain, your medical history, and your lifestyle so we can tailor your care from the start.

2. Choose your clinician
Pick your dedicated physical therapist. They will guide your recovery and adjust your plan as you progress.

3. Start your personalized plan
Using the Sword app, open your personalized care plan and start your recovery. Phoenix, our AI Care Specialist, will guide your progress.
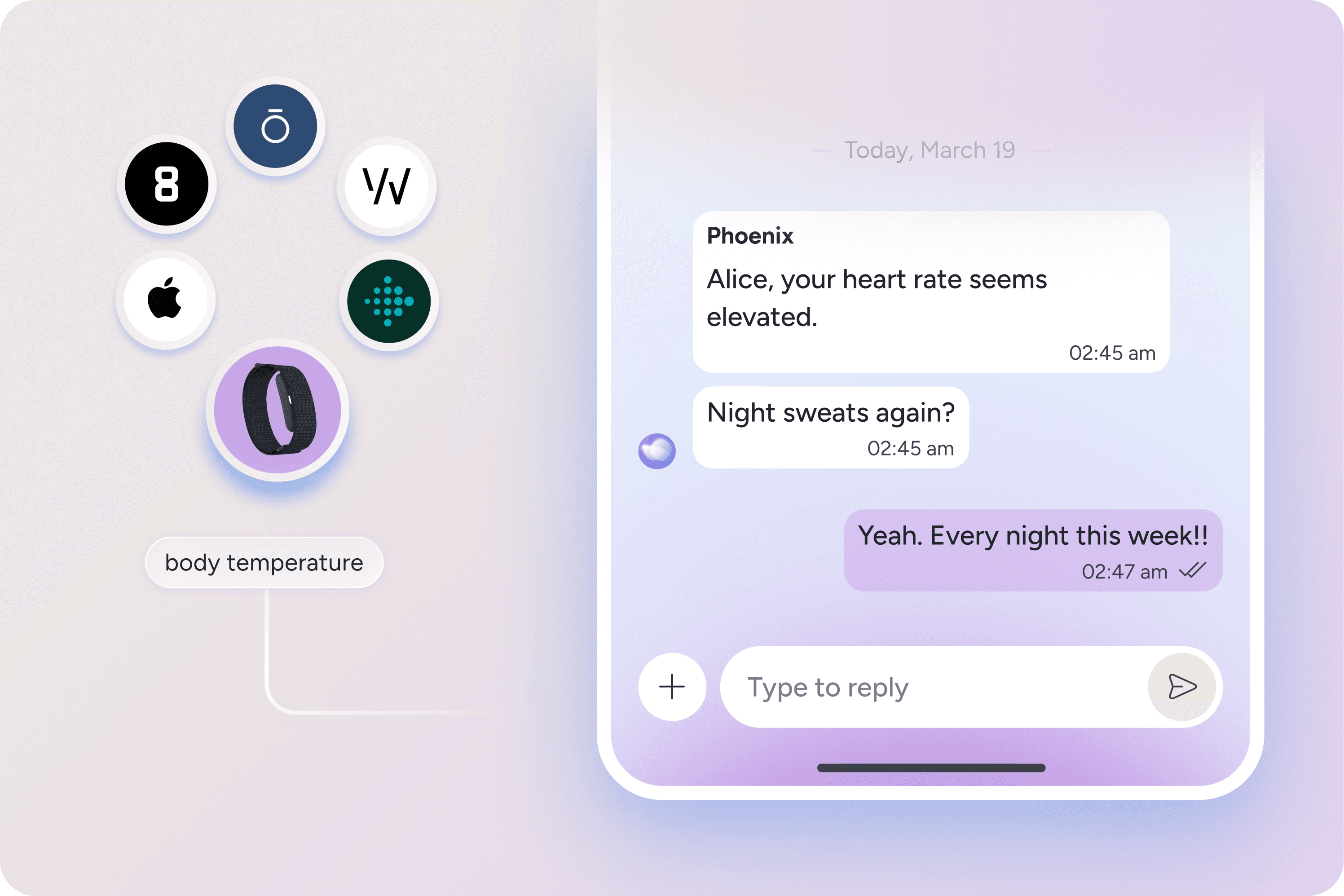
4. Connect your apps for smarter care
Thrive can use your wearable and calendar data to match your routines, key life events, and work patterns to proactively adjust your plan for even better results.
There is good evidence behind this approach. There is also published evidence behind Sword’s digital approach for chronic low back pain. In a randomized controlled trial published in npj Digital Medicine, Sword’s Thrive AI Care program produced improvements in disability and pain that were comparable to evidence-based in-person physical therapy, and the digital group had a significantly lower dropout rate.⁴
Care continues between check-ins, adapts based on your progress, and is available when you need it rather than only when you can schedule it. That structure is also why Thrive members complete their program at a rate of 81%.⁸ Half of the people who start traditional in-person physical therapy stop going after just four sessions. Not because the care does not work. Because the friction of getting there erodes their momentum.⁹
When care fits into your life, you finish it. Thrive user data shows that 69% of all Thrive members are free from limiting pain after completing their care program⁷.

Get back control of your lower back pain and walk freely again
Lower back pain when walking is not something you have to ignore forever. It is a signal that your current movement pattern, load, or recovery capacity may need attention.
The goal is to understand the pain well enough to respond effectively, so walking becomes something you can do with more confidence and less negotiation.
If your pain is limiting your life, it is worth understanding why. If pacing and movement changes are not enough, physical therapy can help clarify what is happening and map out a better next step.
If you are not sure whether Thrive is included in your employer benefits plan, the eligibility check is the fastest way to find out. Check if you're eligible through your employer benefits plan (it takes less than two minutes).

