Pelvic symptoms have a way of shrinking your world quietly.
You may start thinking more carefully about certain workouts or movements. You find yourself keeping track of where the nearest bathroom is. You avoid certain clothes. You brace yourself for coughing and sneezing. You wonder if you are the only one who feels “off” in a way that is hard to name.
If that sounds familiar, you are in the right place. You do not have to accept the symptoms and suffer in silence.
The Sword Summary Warm-up
If pelvic symptoms have made you feel unsure of your body, you deserve an explanation that makes sense and a plan that feels doable.
- Pelvic floor dysfunction is an umbrella term for symptoms that can involve pelvic pain, bladder control, bowel control, pelvic pressure, and sexual comfort.¹
- Pelvic care is often more than “just Kegels,” because pelvic floor muscles may need strength, relaxation, or coordination depending on what is driving symptoms.²
- Pelvic floor muscle training has strong evidence for improving urinary incontinence outcomes for many women when it is taught as a structured program.³
- Like any other muscle in the body, the pelvic floor needs time and consistent practice to change. That’s why many pelvic floor programs recommend practicing regularly for about three months before evaluating progress.⁴
Pelvic floor dysfunction therapy can be an option when you want guided support and a structured plan, but sometimes taking time away from work or family obligations to commute to a clinic can be tough.
If traditional in-person therapy feels hard to access right now, an AI pelvic care program like Bloom can be a practical way to start support at home with one-on-one clinical guidance from a Women’s Health Specialist holding a Doctor of Physical Therapy degree, on your schedule.⁶ No approach is a magic fix. What matters is understanding what is driving your symptoms and following a plan long enough to learn what helps.
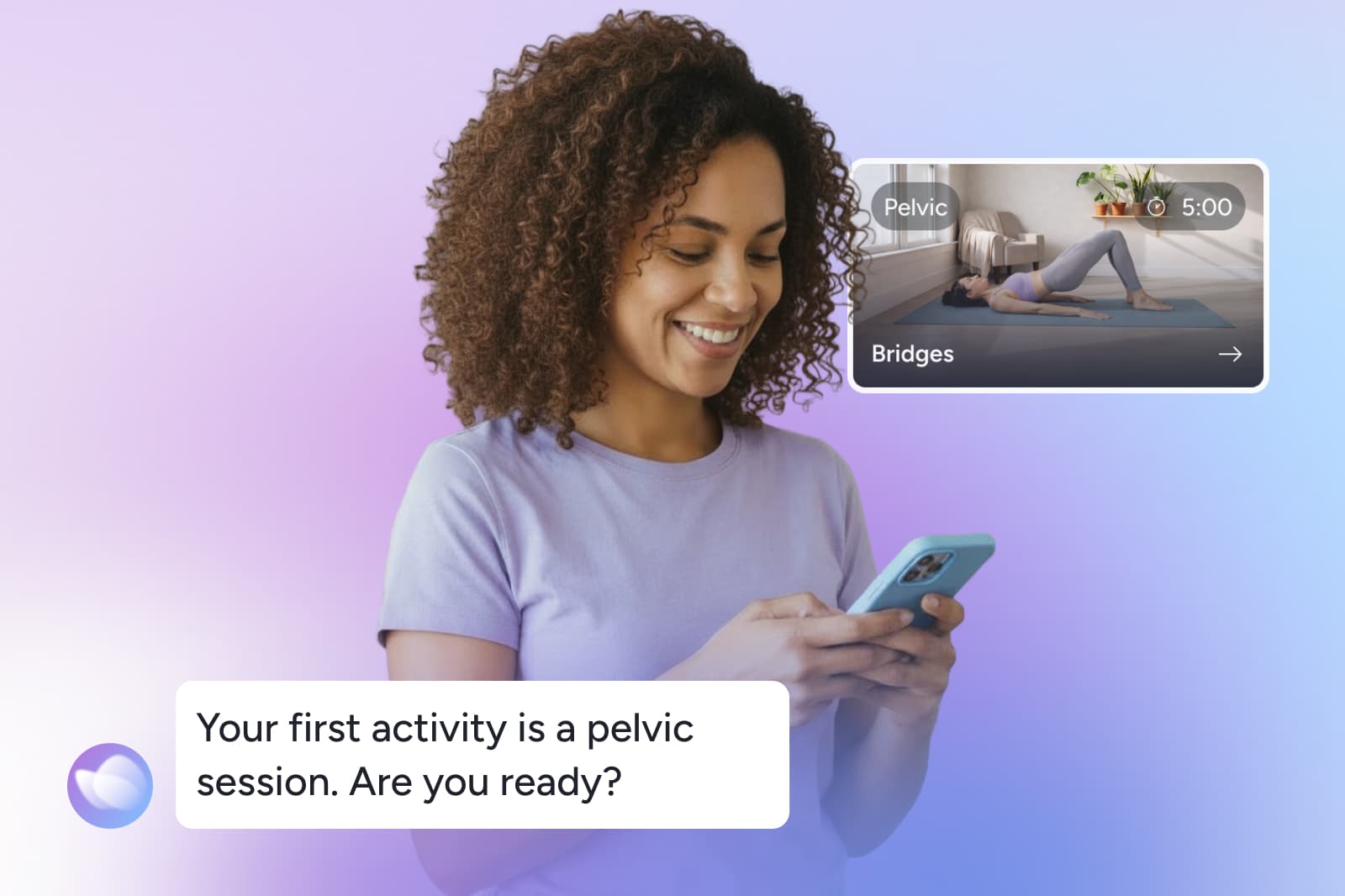
What pelvic floor dysfunction actually means
The pelvic floor is a group of muscles that forms a supportive sling at the bottom of the pelvis. It helps support pelvic organs and contributes to bladder and bowel control and sexual function.¹ ²
“Pelvic floor dysfunction” is a broad label used when those muscles, and the surrounding system, are not working in the way your body needs in that moment.¹ ² That can look different from person to person. It may involve muscles that are underactive and need strengthening. It may also involve muscles that are tight, overworking, or struggling to coordinate and relax.²
Because the pelvic floor supports multiple systems at once, symptoms can show up in different ways depending on how those muscles are functioning.

Common symptoms linked to pelvic floor dysfunction
Pelvic floor symptoms don’t always show up in obvious ways. Because these muscles support the bladder, bowel, and reproductive organs, small changes in how they function can create a wide range of experiences.¹ ² Some people notice one clear symptom. Others experience a mix of issues that seem unrelated at first.
A lot of women learn to normalize pelvic symptoms. Not because they are mild, but because they are private, inconvenient to talk about, and easy to minimize when life is busy. You might tell yourself it is just aging. Or postpartum changes. Or stress. Or something you should be able to “fix” on your own. And just because your mother, aunt, or sisters suffer doesn’t mean you are resigned to dealing with these problems forever.
Bladder symptoms that can change how you plan your day
- Leaking when you cough, sneeze, laugh, lift, or exercise
- A sudden strong urge to urinate that feels hard to hold
- Going “just in case” because you do not trust your bladder
- Waking up at night to urinate more than you want to
Bowel symptoms that can make you feel uncomfortable or “stuck”
- Constipation that keeps coming back
- Straining, even when you are trying to relax
- Feeling like you cannot fully empty your bowels
- Gas leakage or bowel urgency that creates anxiety outside the home
Pressure and support symptoms that are easy to ignore until they aren’t
- A heavy or dragging feeling in the pelvis
- Pressure that worsens after standing, lifting, or a long day
- A bulge sensation that comes and goes
Sexual comfort symptoms that are common, but rarely talked about
- Discomfort with sex, tampon use, or pelvic exams
- Pain that makes you tense up before intimacy even starts
- A feeling of tightness, guarding, or fear of pain
“Whole life” symptoms that pelvic care can influence
- Feeling disconnected from your core after pregnancy or surgery
- Avoiding exercise because jumping, running, or lifting feels risky
- Feeling less confident in your body in public, at work, or while traveling
If these symptoms sound familiar, you’re not alone. Many people begin exploring pelvic floor dysfunction therapy to better understand what’s happening and what support might help.
That is the role Bloom is designed to play. Bloom offers you a personalized digital pelvic care plan that you can access at any time, from the comfort of your home. You get one-on-one clinical guidance from a Women’s Health Specialist holding a Doctor of Physical Therapy degree, available anywhere, anytime, from the comfort of home and on your schedule.⁶
Many pelvic symptoms are signals that your pelvic floor and the surrounding system need support, not silence. Pelvic care is often associated with pain, but that’s only part of the story. Pelvic care can also help with weakness, coordination issues, pressure symptoms, and the day-to-day discomfort that can make you feel less like yourself.
What pelvic floor dysfunction therapy can include
The phrase “pelvic therapy” can sound intimidating if you do not know what it actually involves. Many people imagine a single type of exercise, or assume it will be invasive. In reality, plans vary by setting, but they often follow a few common building blocks. Bloom offers an alternative to pelvic therapy with personalized pelvic care plans that are guided by a matched Women’s Health Specialist (who holds a Doctor of Physical Therapy degree qualification).
Here’s what a clinician may ask about:
- Bladder symptoms (leaks, urgency, frequency, triggers)⁴
- Bowel symptoms (constipation, straining, incomplete emptying)²
- Pressure and bulge symptoms that can suggest prolapse patterns⁵
- Sexual comfort concerns, only to the degree you feel comfortable sharing²
What can you expect from a pelvic care evaluation?
This is the part people worry about most, so it deserves clarity.
In many settings, an evaluation can include movement and breathing assessment, posture or hip mobility checks, and learning how to identify pelvic floor contraction and relaxation.² ⁴ Some clinicians may offer an internal exam because it can provide additional information about coordination or tenderness. That should always be explained clearly, offered as an option, and done only with your consent.
You can ask these questions up front:
- What will today involve, step by step?
- What are my options if I do not want an internal exam?
- How will we measure progress over time?⁴
You are allowed to pause, skip, or stop any part of the process. A good plan is both effective and respectful, and should adapt to your needs and preferences.
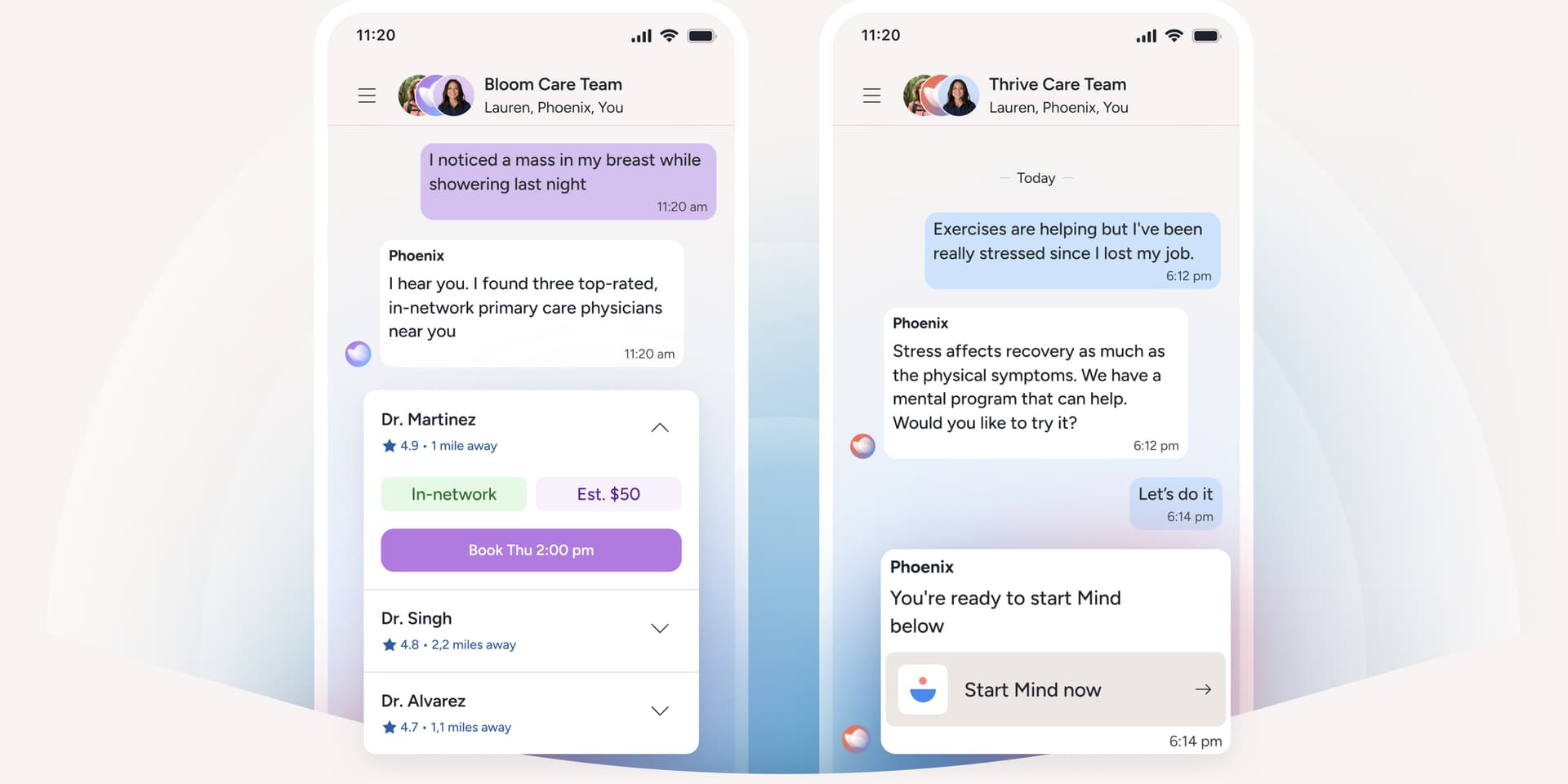
Bloom helps you manage pelvic floor dysfunction from the comfort of home
For people who want support that fits real life, Bloom is a purpose-built women's health AI Care program with one-on-one clinical guidance, available anywhere, anytime, from the comfort of home and on your schedule.⁶
When therapy requires you to rearrange your whole life, it becomes easy to postpone. When support fits into your actual week, it becomes easier to start and to stay consistent long enough to see change.
Bloom is built to be safe and discreet. It is also designed to move you from “I tried some exercises” to a structured plan that matches your symptoms and progresses over time.⁶
What to expect from Bloom
How Bloom supports you, step by step
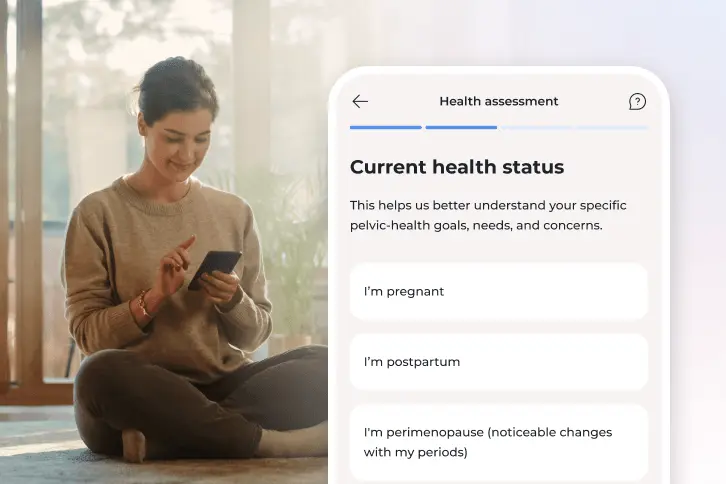
1. Tell us what you’re experiencing
Share your symptoms, goals, and what you need support with so Bloom can tailor your plan.

2. Meet your Women’s Health Specialist
Match with a Women’s Health Specialist who holds a Doctor of Physical Therapy degree and helps guide your plan.
3. Receive your Bloom kit
We’ll send everything you need, including the Bloom Pod, directly to your door.
4. Start guided sessions from home
Use Bloom privately from home with real-time feedback and 24/7 support along the way.
Get your own personalized Bloom pelvic care plan
You do not need to wait until symptoms are “bad enough” to deserve support. If your daily choices are changing because of pelvic symptoms, that is enough.
If you want private, flexible support that meets you where you are, Bloom offers digital pelvic care with one-on-one clinical guidance from a Women’s Health Specialist holding a Doctor of Physical Therapy degree, available anywhere, anytime, from the comfort of home and on your schedule.⁶
Many employers and health plans offer Bloom as a covered health benefit. Checking eligibility takes less than two minutes. If you are covered, you can begin your personalized program within days. Check your eligibility now to confirm your access and take the first step from home, on your schedule.

