Some women describe postmenopausal pelvic discomfort like a dull heaviness, a dragging sensation, or a “fullness” that makes it hard to get comfortable. Others notice dryness, burning, urinary urgency, or discomfort during or after sex.
When symptoms feel private or hard to describe, it is easy to minimize them and adapt your life around them. That pattern is common, and it is also exhausting.
You do not have to accept pelvic discomfort as the price of getting older. This is a common experience, and understanding what might be driving it can help you choose a care option that feels realistic and reassuring.
The Sword Summary Warm-up
Don’t have time for the full workout? We’ve got you covered with a quick, high-intensity session. Here are the key takeaways:
- Postmenopausal pelvic discomfort can include heaviness, pressure, dryness, burning, urinary changes, or pain with sex.¹ ²
- These symptoms often go unaddressed because they feel private or difficult to describe, and many women are reluctant to seek traditional care.
- Two common drivers are genitourinary syndrome of menopause (GSM) and pelvic organ prolapse, both more common after menopause.¹ ²
- Support often starts with symptom-specific basics (comfort strategies, bladder and bowel habits, and guided pelvic floor training) plus medical evaluation for red flags like postmenopausal bleeding.¹ ³ ⁴
- A dedicated care program from Sword Bloom can make it easier to start privately at home, with one-on-one clinical guidance from a Women’s Health Specialist holding a Doctor of Physical Therapy degree.⁵ ⁶
What does postmenopausal pelvic discomfort feel like?
Pelvic discomfort is a wide umbrella. You might notice one symptom, or several at once.
- Heaviness, pressure, or a dragging feeling in the pelvis²
- A bulge sensation in the vagina, or feeling like “something is coming down”²
- Vaginal dryness, irritation, burning, or pain with sex¹
- Urinary urgency, more frequent urination, burning with urination, or recurrent urinary symptoms¹
- Constipation or feeling like you cannot fully empty your bowels²
Take a simple refresher on the basics of pelvic floor function, and this context can make these symptoms feel less mysterious and easier to talk about.
Common causes of postmenopausal pelvic discomfort
Pelvic symptoms after menopause are not always caused by one single issue. Often, it is a combination of tissue changes, muscle coordination, and everyday pressures on the pelvic region.
Genitourinary syndrome of menopause

Genitourinary syndrome of menopause (GSM) is a medical term that includes vaginal and urinary symptoms related to lower estrogen levels after menopause.¹ The North American Menopause Society notes GSM is common, with estimates ranging from about 27% to 84% of postmenopausal women.¹
Symptoms often include vaginal dryness, burning, irritation, pain with sex, and urinary symptoms like urgency or discomfort with urination. GSM symptoms also tend to persist and worsen if women don't access care. This is why “waiting it out” often leaves people stuck in the same cycle.¹
If GSM sounds like what you are experiencing, it can help to know this upfront: you can find care options that are private and easy to access. Bloom offers dedicated support for women in menopause with personalized care plans that are accessible from the comfort of home with 24/7 access via the Sword app. Also, women's health clinicians can help you review what is going on, rule out other causes, and talk through approaches that match your symptoms and preferences.¹
Pelvic organ prolapse

Pelvic organ prolapse can happen when pelvic floor support changes and pelvic organs shift downward. That can create a feeling of heaviness, pressure, or a bulge in the vagina.² Symptoms can also include urinary issues, bowel problems, and discomfort during sex.²
Prolapse is common after menopause and it is also highly variable. Some people have mild symptoms that come and go. Others notice symptoms more at the end of the day, after lifting, or after standing for a long time.²
If you want a deeper explanation of symptoms and guided support options, this prolapse guide walks through what to look for and what options exist.
Pelvic floor dysfunction and tension patterns

Sometimes discomfort is not only about weakness. Many women report feeling joint pain and muscle aches after menopause, likely from overworking, holding tension, or struggling to coordinate the pelvic floor. That can contribute to symptoms like pelvic pressure, incomplete emptying, constipation and straining, or pain with penetration.
This is why the best support plans look beyond “just do Kegels” and focus on coordination, relaxation, pressure management, and habits that keep symptoms looping.
What you can do now to feel more comfortable
Before assuming surgery is the only solution, it’s worth starting with conservative strategies that can reduce strain on the pelvic floor and may help improve symptoms. These steps are not meant to replace medical guidance. They can help you feel more comfortable while you decide what support makes sense.
Reduce irritation and support vaginal comfort
If dryness or irritation is part of your discomfort, first step is to discuss any GSM-specific options with a clinician, because effective treatments are available.¹ The clinician may suggest a vaginal moisturizer used consistently and the application of a water-based lubricant during sex. These treatments can help many women feel more comfortable.¹
Support bladder and bowel habits that reduce pelvic strain
Bladder urgency and constipation can both increase pelvic pressure. Small changes may help, such as:
- Stay hydrated and aim for regular fiber intake.
- Avoid straining by using a footstool to support a more comfortable toileting posture.
- Try to respond to true bladder cues rather than going “just in case” all day.
Use gentle movement and pressure awareness
Long periods of sitting or standing can increase heaviness for some women. Short walks, gentle mobility, and learning how to exhale during effort (instead of holding your breath and bearing down) may reduce pelvic pressure over time. If you want a practical starting point, these pelvic health tips can act like a doable habits checklist.
When pelvic discomfort needs medical evaluation
Most pelvic discomfort after menopause has non-emergency explanations, but some symptoms should be checked promptly. Seek medical evaluation if you have any of the following more severe symptoms:
- Any bleeding after menopause, even spotting³
- New or intense pelvic pain, fever, or feeling very unwell
- Pain with urination plus fever or flank pain
- A bulge that is painful, worsening quickly, or associated with difficulty urinating or passing stool
Recover at home with 24/7 access to a personalized Bloom care plan
Once you have a sense of what symptoms you are dealing with, the next question is usually practical: what is the easiest way to get guided support without adding more stress to your schedule?
Bloom is digital pelvic care, available anywhere, anytime, from the comfort of home and on your schedule. It offers expert pelvic care with one-on-one clinical guidance from a Women’s Health Specialist holding a Doctor of Physical Therapy degree.⁵
Bloom is designed for the reality that women’s health symptoms can feel private, and logistics can make in-person care hard to access consistently. The goal is to make it easier to begin with a plan built around your symptoms and your life.⁵
What to expect from Bloom
How Bloom supports you, step by step
1. Tell us what you’re experiencing
Share your symptoms, goals, and what you need support with so Bloom can tailor your plan.

2. Meet your Women’s Health Specialist
Match with a Women’s Health Specialist who holds a Doctor of Physical Therapy degree and helps guide your plan.
3. Receive your Bloom kit
We’ll send everything you need, including the Bloom Pod, directly to your door.
4. Start guided sessions from home
Use Bloom privately from home with real-time feedback and 24/7 support along the way.
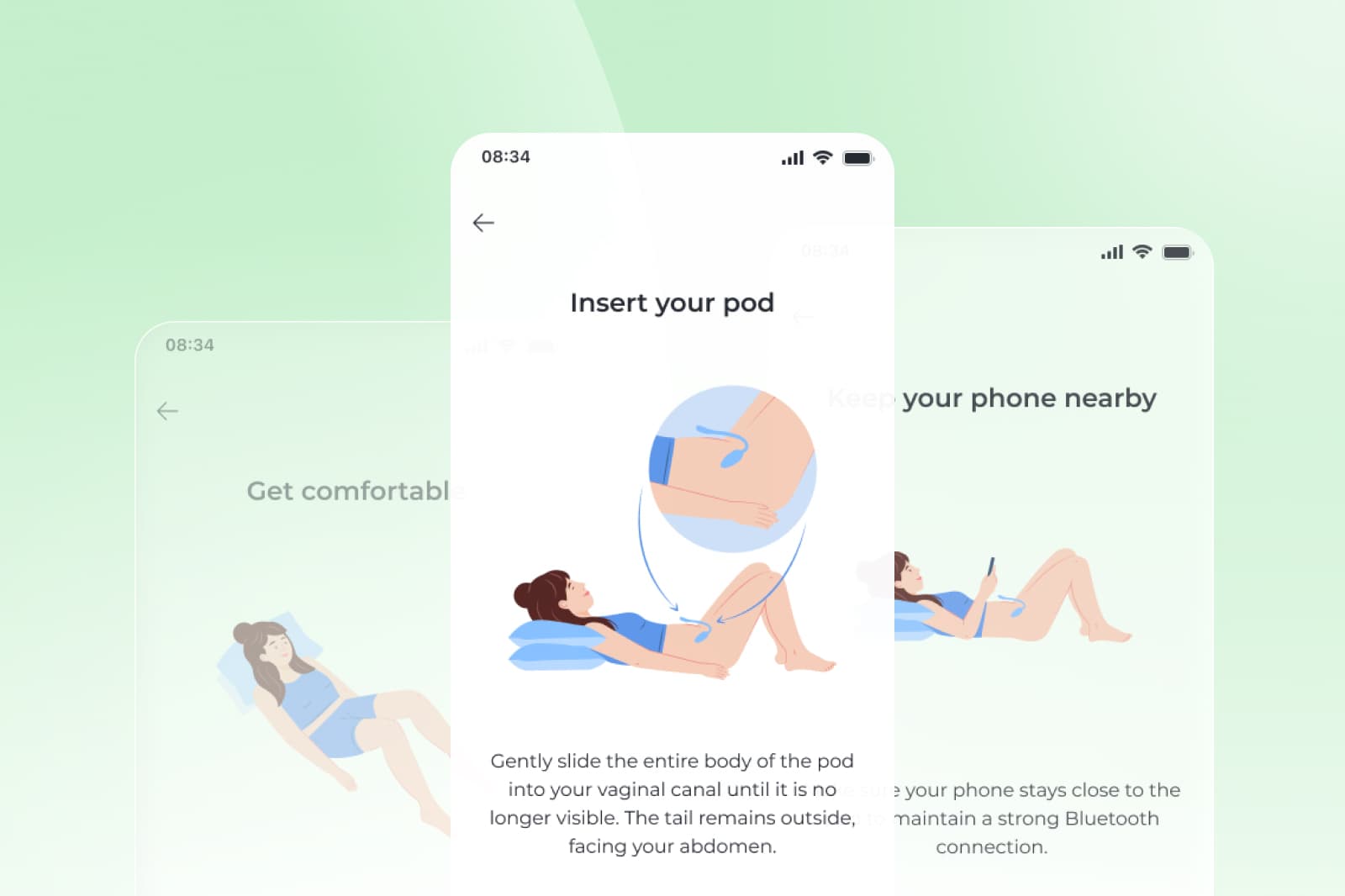
For many members, a key part of the experience is real-time feedback during sessions through the Bloom Pod, an intravaginal sensor that works with the Sword app to support pelvic floor contraction and relaxation practice.⁶ Bloom also includes guidance from your matched Women's Health Specialist on when symptoms suggest seeking in-person medical evaluation.⁵
How the Bloom Pod supports and strengthens the pelvic floor muscles
When working on recovery exercises, many women wonder the same thing: Am I even doing the exercises correctly? That uncertainty is one of the most common reasons women don't finish prescribed care plans or never start at all.
The Bloom Pod is an intravaginal sensor that pairs with the Sword app and provides real-time feedback during guided sessions.⁶ The goal is not intensity. It’s confidence and precision: helping you practice pelvic floor contraction and relaxation in a way that is easier to understand and repeat.⁶
For members who feel unsure about whether they’re engaging or relaxing the pelvic floor effectively, this feedback can make the work feel more concrete and less like guesswork.⁶
Get expert care from the comfort of home with Bloom
Postmenopausal pelvic discomfort is personal. That’s exactly why the support should feel private, respectful, and easy to begin.
Bloom is designed to let you start from home, with a personalized care plan that fits your schedule.⁵ It’s a way to move from “I’m just dealing with this” to “I have support, and I know what to do next,” without adding another logistical burden to your life.
Bloom’s results speak for themselves:
- 65% of women report meaningful improvement in daily life¹⁵.
- 56% experience higher productivity and 50% report less anxiety¹⁵.
- 77% complete their program, exceeding typical in-person adherence rates¹⁶.
These outcomes show that consistent, guided pelvic care can reduce your symptoms, prevent discomfort, and rebuild your body confidence from the privacy of home. You get 24/7 access to your personalized care plan and direct support from your matched women's health expert through the Sword app.
Many employers and health plans offer Bloom as a covered health benefit. Checking eligibility takes less than two minutes. If you are covered, you can begin your personalized program within days. Check your eligibility now to confirm your access and take the first step from home, on your schedule.

