July 24, 2025
GLP-1 and lean mass loss: your members need structured support plans
Up to 39% of weight lost during GLP-1 treatment can come from lean mass. Learn how to reduce the risk with structured support that helps protect your GLP-1 spend and member outcomes.
Written by

Head of Clinical Strategy, Sword Pulse
GLP-1 medications are having a strong and fast impact. Patients are losing weight and in the short term, results are positive.
These medications work effectively to promote fast weight loss by curbing appetite, slowing gastric emptying, and improving glycemic control. The possibility of delivering these outcomes without stimulants or surgery represents a significant step forward for obesity treatment.
However, employers and insurers need to make sure that GLP-1 use is supported by structured lifestyle support over time. One clinically significant issue in particular often goes unnoticed...
GLP-1-induced lean mass loss is a hidden danger
The cost of muscle loss can be significant for patients and health insurers alike. Up to 39% of lean muscle mass is lost during GLP-1 medication usage.1
Muscle loss often goes unnoticed during GLP-1 treatment programs and this won’t show up in pharmacy claims.1
- Lean muscle loss is rarely coded as a primary condition. Sarcopenia (a condition characterized by progressive loss of skeletal muscle mass and strength)¹⁵ is underdiagnosed in clinical settings, particularly when it is medication-induced or occurs in non-elderly populations₅.
- Patients are unlikely to monitor this risk factor. However, the downstream impact of lean muscle loss is significant and serious, leading to an increased risk of musculoskeletal conditions.¹⁵
- Sedentary GLP-1 users are at higher risk. Without structured physical activity or strength training, muscle atrophy can occur gradually. This secondary effect is likely to go unnoticed as the required strength assessments or body composition testing are rarely practiced.¹⁴
The good news is this risk can be miinimized. GLP-1 prescriptions can be supported by structured programs like Sword Pulse that help people build strength, maintain activity, and develop habits that protect against lean-mass loss over time.
How GLP-1s contribute to lean mass loss
GLP-1 medications mimic a hormone that helps regulate hunger and digestion. By reducing appetite and slowing the rate of digestion, patients tend to eat smaller portions and less frequently. This leads to a significant reduction in calorie intake, contributing to weight loss observed on the scale.₁
Importantly, not all weight lost is fat. GLP-1-related weight loss is not always fat-only. Without support to help preserve muscle, both fat mass and lean mass may be lost during treatment.¹
The risk may be higher for individuals who are already sedentary, especially if they do not have established habits of regular physical activity². Fewer than 1 in 4 U.S. adults meet CDC guidelines for aerobic and muscle-strengthening activity.2
Most of your existing members aren’t moving enough to retain muscle when they begin to lower their calorie intake. A snapshot analysis of the Sword Move population shows this risk factor is widespread³:
- 76% of Pulse members are overweight or obese
- 57% have an addressable health condition such as diabetes, high cholesterol, or a similar condition
- 46% had low physical activity at baseline
The takeaway learning for insurers and employers with GLP-1 spend is clear. Prescriptions should be supported by structured movement plans to ensure patients engage in regular physical activity and to prevent muscle loss.
Why lean muscle mass retention is critical for sustained weight loss
Muscle loss adds nearly $900 in excess healthcare costs per employee annually4. So what’s happening in the patient’s body that leads to these huge downstream costs?
Lean muscle mass includes metabolically active tissue that powers movement needed for daily life and underpins long-term health.
How lean muscle protects the body
- Supports joint integrity and reduces stress on the musculoskeletal system⁴
- Helps protect balance, coordination, and fall resilience⁶
- Supports resting metabolism and glucose regulation⁸
- Helps maintain functional independence in daily life⁸
When muscle is lost during weight loss programs (especially if fat is regained after discontinuation) patients often end up with worse body composition¹ and increased cardiometabolic and musculoskeletal risk⁴. This reversal undermines the original goals of weight loss, both clinically and financially.
Research shows that muscle mass plays a protective role across multiple systems in the body, from maintaining metabolic health to preventing MSK pain and instability.⁴ When GLP-1 users lose lean mass, they also lose strength, balance, and resilience. All of these attributes are crucial for function and injury prevention.
Muscle loss over a broad member population often leads to serious risks and costs
- Higher musculoskeletal risk from pain and overuse-related issues⁵
- More fall-related injuries and disability exposure⁶
- Lower odds of maintaining results if strength and function decline¹⁶
- Greater risk that early success becomes harder to sustain over time⁹
The resulting downstream costs including physical therapy, imaging, medication, and even surgical interventions, are often preventable with proactive lean mass preservation strategies.⁴
The clinical risks of GLP-1 lean mass loss
Lean mass loss isn’t just a side effect. It’s a predictive risk factor for costly, preventable conditions. Clinical research shows:
- up to 33% of chronic pain cases in older adults⁵
- a 60% higher risk of falls⁶
- a 2.5x higher disability risk in people with sarcopenic obesity⁷
These risks impact return-to-work timelines, independence in daily life, long-term physical therapy and imaging spend, and claims exposure associated with related conditions.⁵ ⁷
Unfortunately these incidences are rarely connected back to lean muscle mass loss during GLP-1 treatment.
GLP-1 lean mass loss doesn’t always show up in claims
Lean tissue degradation doesn’t have a neat ICD-10 code. But the effects ripple across data sets:
- Members who lose weight but develop new MSK pain₉
- Increases in fall-related ER visits among previously low-risk members⁶
- Energy decline and functional loss despite weight loss⁴
- Reduced success with activities of daily living, particularly in regular tasks like climbing stairs, rising from chairs, or carrying groceries⁴
Perhaps the most expensive risk factor is re-prescription of GLP-1s.
This can happen as patients experience poor functional retention, with studies showing that functional decline can limit patients’ ability to maintain weight loss without ongoing medication.⁸
GLP-1s may help with short-term weight loss, but if they erode lean muscle mass, joint health and patient stability, the dangers of this long-term deterioration start to outweigh the benefits.
Movement is the proven path to preserve lean mass
Structured, strength-building movement is one of the most evidence-supported ways to help protect lean tissue during pharmacological weight loss.¹⁴ That means:
- Resistance training that builds or maintains muscle
- Progressive overload tailored to individual fitness and condition
- Wearable integration for adherence and safety
- Clinical oversight for accountability
Without this, lean GLP-1 patients risk the serious dangers of lean muscle loss. In addition, one of the biggest concerns with GLP-1 use is sustainability. So many people rebound to old habits, with as many as two-thirds of lost weight may be regained after stopping treatment.⁹
Prescribing structured movement plans to support GLP-1 medication helps to develop positive behavior change and establish a physical activity routine. These regular movement patterns allow the patient to retain lean muscle mass even when calorie intake is lowered and weight is lost.¹⁴
What progress can look like with Pulse
Pulse supports GLP-1 users with continuous lifestyle support built around strength, nutrition guidance, and daily habits:
- 83% of members report feeling better or much better3
- 51% of members with low physical activity at baseline reached the World Health Organization recommended activity threshold after 27 days of Pulse sessions3
These signals do not prove every downstream outcome on their own. But they do show the kind of sustained engagement needed to make GLP-1 results more durable over time with:
- Lower MSK claims¹²
- Better functional outcomes¹³
- Improved GLP-1 satisfaction and adherence¹³
- Fewer re-prescriptions and better long-term outcomes⁸
How Pulse supports GLP-1 users
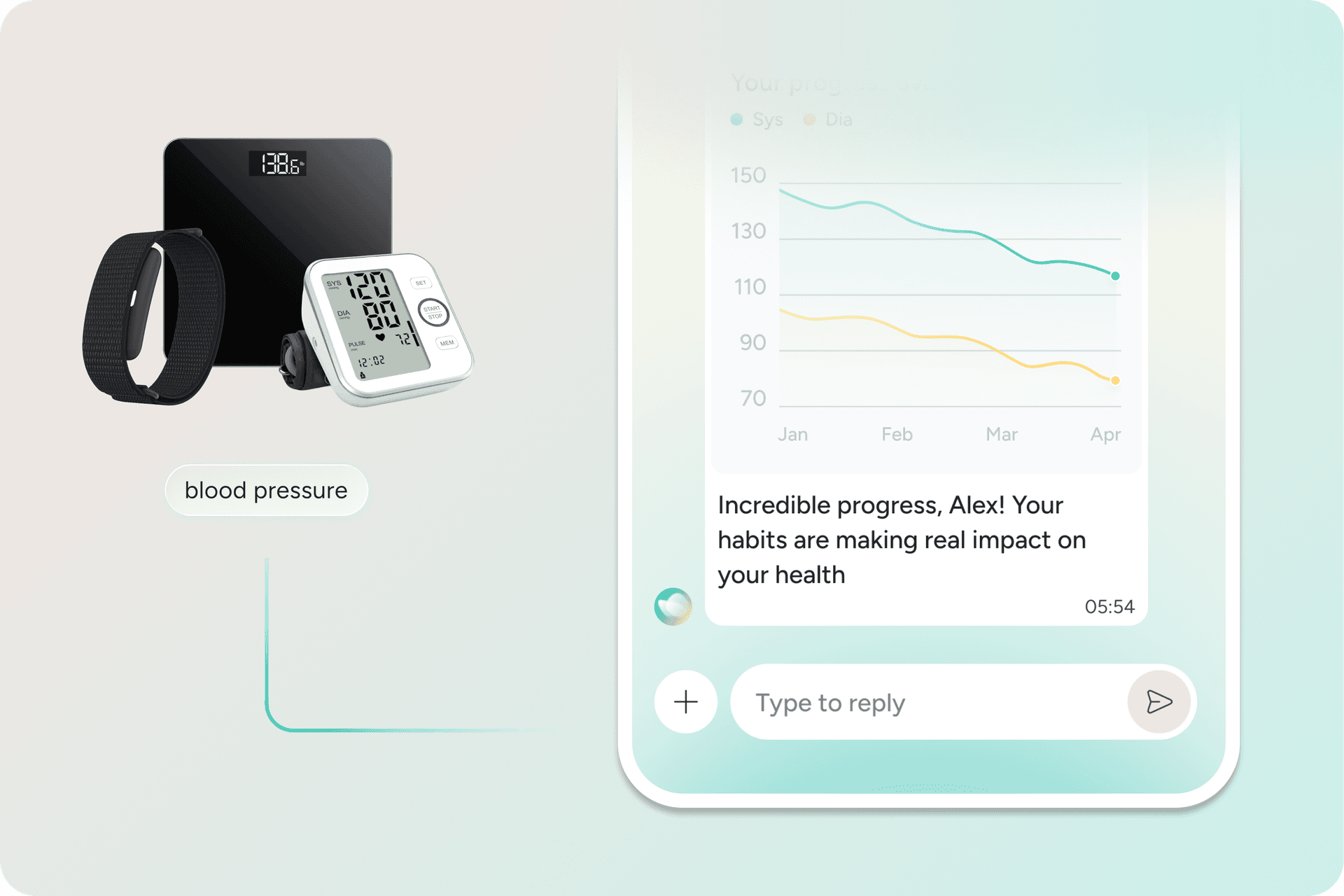
Pulse is the cardiometabolic pillar of the AI Care Platform. For GLP-1 users, Pulse is designed to address what medication alone does not: muscle preservation, strength-building support, nutrition guidance, and the daily habits that help results last.
Pulse provides GLP-1 wraparound care that helps members preserve muscle, build strength, and develop healthier routines alongside medication use. The goal is not to replace the prescription. It is to support the parts of the journey medication does not cover on its own.¹⁸ Each Pulse member receives:
- Personalized support across movement, nutrition, and daily habits
- Ongoing engagement from Phoenix, Sword Health’s AI Care Specialist
- Guidance from a matched Health Specialist when nuance or clinical judgment matters
- Connected-device support, including blood pressure monitors, smart scales, and wearables where appropriate
- Reporting tied to engagement and measurable improvement
This kind of continuous support is especially important for GLP-1 populations, where success depends not only on weight loss, but on whether members maintain strength, function, and habits over time.
What's next for fast and effective implementation
To maximize your GLP-1 investment and protect against downstream cost exposure, leading employers and health plans are taking action now. Here’s how to build a more sustainable, outcomes-focused care model:
- Conduct a retrospective MSK audit. Identify claims 6–12 months post-GLP-1 initiation, especially related to pain, falls, or functional loss.
- Flag high-risk members. Look for those with rapid weight loss, sedentary baseline activity, or new MSK complaints.
- Implement structured wraparound support. Build movement, strength, and habit support into your GLP-1 benefit design.
- Track functional outcomes. Partner with vendors who measure more than weight: activity level, strength, stability, and daily functioning.
Strengthen the long-term value of your GLP-1 strategy
GLP-1s can support weight loss, but they do not protect muscle or create sustainable habits on their own. Pulse helps fill that gap with structured cardiometabolic support built around strength, nutrition guidance, and day-to-day behavior change.
Build a more sustainable healthcare strategy
See how Sword Health helps employers address rising healthcare costs with outcomes-based care across high-cost populations.
Footnotes
- 1
Prado, Carla M. et al. The Lancet Diabetes & Endocrinology, Vol. 12, Issue 11, 785–787
- 2
Elgaddal N et al. "Physical activity among adults aged 18 and over: United States, 2020." NCHS Data Brief No. 443, 2022. https://dx.doi.org/10.15620/cdc:120213
- 3
Sword member base, 2025, proprietary.
- 4
Janssen I et al. "The healthcare costs of sarcopenia in the United States." Clinical Interventions in Aging. 2017;12:517–528.
- 5
Hicks GE et al. Pain Medicine. 2004;5(2):125–134.
- 6
Sousa AS et al. Clinical Nutrition ESPEN. 2022;50:63–73.
- 7
Baumgartner RN et al. Obesity Research. 2004;12(12):2061–2070.
- 8
Tamborlane WV et al. Journal of Managed Care & Specialty Pharmacy. 2024;30(5):540–548.
- 9
Wilding JPH et al. Lancet Diabetes & Endocrinology. 2022;10(12):873–885.
- 10
Validation Institute. Pulse delivers a 3.1x return on investment and $1,663 in average annual savings per member
- 11
Sword Health. Member reassessment data, 5+ weeks. Internal data.
- 12
Sword Health. Move Book of Business, H1 2024. Internal data.
- 13
Sword Health. PGIC scores, 2023–2024. Internal data.
- 14
American College of Sports Medicine. "Position stand: progression models in resistance training for healthy adults." Medicine & Science in Sports & Exercise. 2009;41(3):687–708.
- 15
Cruz-Jentoft AJ et al. "Sarcopenia: revised European consensus on definition and diagnosis." Age and Ageing. 2019;48(1):16–31.
- 16
Magkos F et al. “Skeletal muscle loss during weight loss.” Nature Reviews Endocrinology. 2023;19:321–334. https://doi.org/10.1038/s41574-023-00885-z