Sword Summary Warm-up
Don’t have time for the full workout? We’ve got you covered with a quick, high-intensity session. Here are the key takeaways:
- Most MSK pricing conversations focus on unit price and miss the real problem: it's the pathway that drives cost, not any single service.
- Reference-based pricing can reduce unit price variation but does nothing to stop low-value escalation once a member is already in a high-cost pathway.
- Outcome-based pricing changes the financial signal: payment follows verified improvement, giving finance teams billing they can forecast and defend.
- Predictive models close the gap that payment models alone cannot: they identify which members are heading toward high-cost care early enough to change the trajectory.
The RFP that never quite answered the question
Every MSK vendor in your last RFP said they deliver outcomes. Some had slides with completion rates. Others had ROI figures. A few had outcome-based pricing language somewhere in the contract summary.
And yet, when the QBR arrives six months later, you're still trying to explain why the MSK line moved and whether the program actually changed what happened next for members.
The problem isn't that vendors are dishonest. It's that most MSK pricing models answer the wrong question. They tell you what a service costs. They don't tell you whether buying that service changed the trajectory of a member's care, or what happens when it doesn't.
There are three models worth understanding before your next MSK contract. Each answers a different question. Each has a different failure mode. And knowing the difference before the RFP goes out is worth more than any amount of negotiating afterward.
A simple way to compare the models
Before getting into each one, here is how they stack up on what finance and benefits leaders actually need to manage MSK spend:
| Model | What it controls | What it often misses | Best use case |
|---|---|---|---|
Reference-based pricing | Unit price | Pathway escalation | Narrowing price variation |
Outcome-based pricing | Payment tied to improvement | Needs good measurement ops | Clear accountability and forecasting |
Predictive models | Targeting and early intervention | Must be transparent to earn trust | High-risk populations, in-year impact |
Model 1: Reference-based pricing
Reference-based pricing is where most buyers start. You set a benchmark for allowed amounts, often Medicare-based, and negotiate around that anchor. It reduces extreme price variation and it makes procurement conversations feel more concrete when you can point to a schedule.
The catch for MSK is that reference pricing answers the wrong question.
- It tells you whether you overpaid for a service.
- It does not tell you whether the service was the right one, or whether the member needed it at all.
If the care pathway is still imaging-first and procedure-forward, reference-based pricing just means you pay fair prices for low-value escalation. The spend is still unpredictable because the incentives driving utilization haven't changed.
Think of it as a floor, not a strategy. It's worth having but it won't solve the forecasting problem on its own.
Model 2: Outcome-based pricing
Outcome-based pricing starts from a different premise. If the goal is improvement, payment should require improvement. That sounds obvious. It's still rare in practice because it requires two things most models quietly avoid: a clear definition of what improvement means, and a payment rule that actually follows that definition.
When it works, it does something finance teams recognize immediately:
- Claims volatility gets replaced by contractual triggers.
- You know in advance what will be billed and when.
A contract built around genuine outcome accountability typically includes a validated outcome measure named explicitly in the agreement, an explicit threshold that defines success, billing triggers and non-triggers that are unambiguous, and reporting that reconciles outcomes to invoices rather than just describing them.
Sword's Outcome-based pricing is built on exactly this structure. Payment is split in two milestones:
- 50% at activation and
- 50% only when a member achieves meaningful improvement, measured using PGIC (Patient Global Impression of Change). ³ ⁵
PGIC asks members how they feel compared to when they started care. Sword uses a score of 5 or above as the success threshold, and that threshold sits in the contract.¹ ⁵
The test for any outcome-based contract is simple: can the vendor show you, in the contract itself, exactly what gets billed and what doesn't when a member doesn't improve? If they can't answer that clearly, the accountability is in the pitch deck, not the agreement.
Model 3: Predictive models
Even a well-designed payment model can only govern what it can measure. Predictive models solve for a different gap: they identify which members are on a path toward high-cost care early enough to intervene before the escalation becomes a claim.
In MSK, most of the biggest savings opportunities come from preventing the expensive branch of the care pathway, not from optimizing the cheaper one. A member who gets into conservative care before they're referred for imaging or surgery is a fundamentally different financial story than one who doesn't.
A credible predictive model should be transparent about what it's targeting and why, how signals are validated, how selection bias and fairness are monitored, and how the targeting connects to actual outcomes measurement. The moment a predictive model feels like a black box, it creates exactly the kind of trust problem that undermines the whole program.
The strongest designs layer predictive targeting on top of outcome-based payment: early identification focuses effort where it matters, and outcome-based billing ensures the effort is still accountable. Both the pathway and the payment rules become more structured, and forecasting improves accordingly.
Consider the pricing model that fits your situation
Most buyers don't have to choose just one. The three models address different problems and the most defensible MSK strategies usually combine more than one layer.
- If your primary problem is unit price variation, reference-based pricing creates a useful floor. Treat it as a control, not a strategy.
- If your primary problem is ROI defensibility and forecasting, outcome-based pricing gives you the clearest signal because payment follows a defined improvement threshold you can verify.
- If your primary problem is in-year impact in a population you know has high-risk members, predictive targeting focuses intervention where escalation is most likely before it hits your claims.
8 questions to separate a pricing model from a pricing story
Before any MSK contract, these questions reveal more than any feature walkthrough:
- What exactly triggers a payment, and what explicitly does not?
- What outcome measure defines success, and why that measure?
- What threshold counts as meaningful improvement?
- How is missing outcome data handled, and how does that affect billing?
- Can you show a sample report that reconciles outcomes to invoices?
- Where, specifically, does the model reduce low-value escalation?
- If predictive targeting is used, how is it validated and monitored for fairness?
- What protections exist for budget exposure?
If a vendor can't answer these in the contract language itself, you're evaluating their sales story, not their accountability model. This value-based contracting checklist covers all of these in full, with context for each clause.
The buyers who ask these questions before signing fare better
The buyers who get the most out of outcome-based MSK contracts are not the ones who negotiate the hardest on price. They're the ones who read the contract carefully enough to ask what happens when a member doesn't improve.
That question, asked before you sign, is worth more than any ROI claim in the pitch. It is the moment the conversation moves from pricing story to pricing model.
Book a demo to see how Sword's contract mechanics answer it.
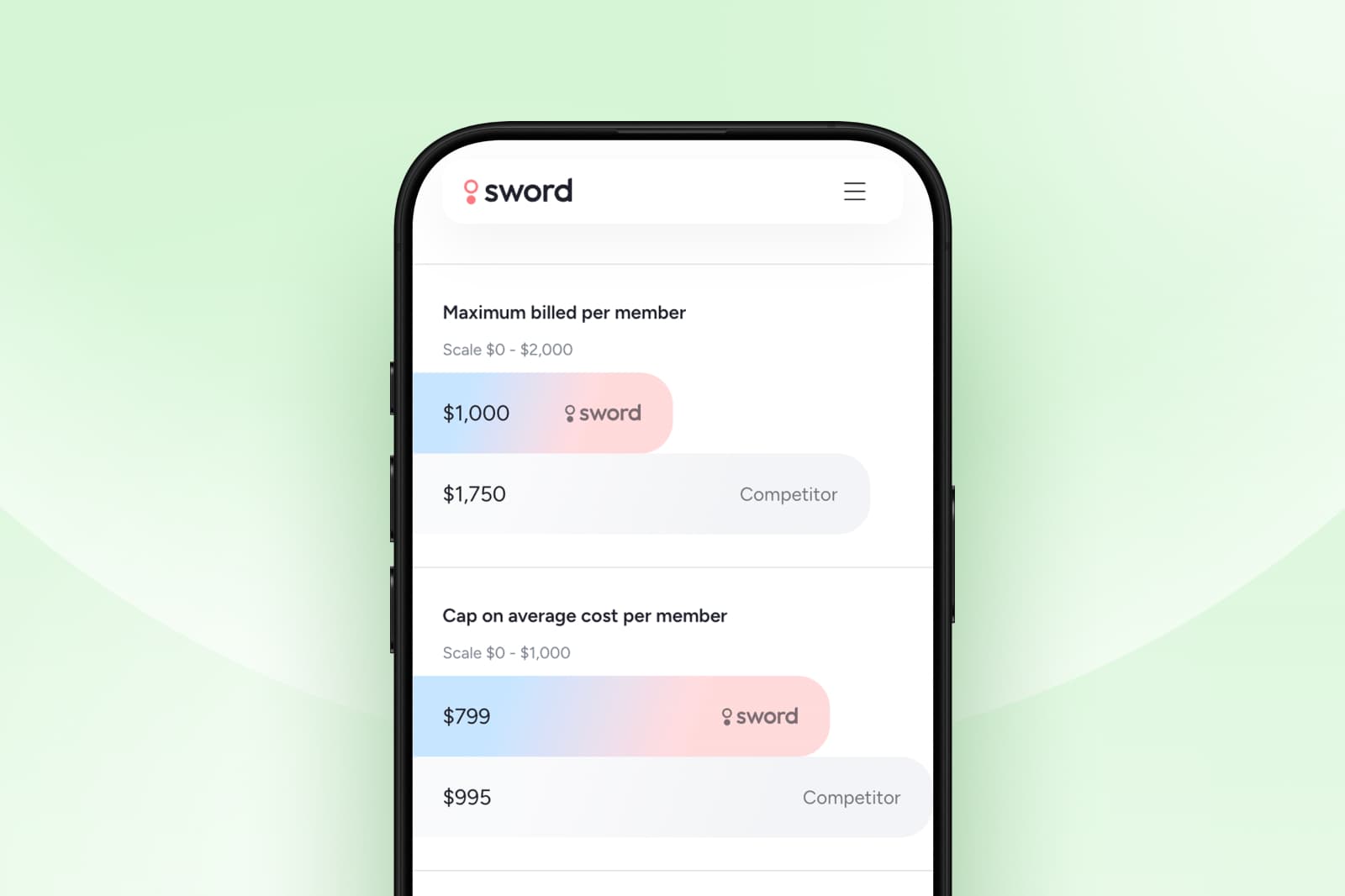
GUARANTEED SAVINGS
Get the industry's highest ROI and slash MSK spend with Sword
3.2x
Average ROI (the industry's highest independently-validated rate)
70%
reduction in surgery intent
41%
fewer ancillary services
10%
drop in MSK-related MRIs
35%
reduction in spine surgeries
