Weight loss drugs are rewriting the obesity care playbook. GLP-1s like semaglutide, liraglutide, and others are helping members lose weight, improve metabolic markers, and avoid high-risk interventions like surgery.
Many employers and health plans have fast-tracked these medications into formularies as a cornerstone of chronic condition management. But there’s one effect that most treatment programs overlook and it’s not related to fat loss. It’s about muscle loss.
Research suggests that up to 39% of weight lost during GLP-1 use may come from lean mass.¹ That can increase downstream risk around fatigue, falls, musculoskeletal issues, and higher-cost utilization over time.
The silent risk in your obesity care strategy
This is more than a side effect to monitor. Muscle loss is a systemic risk that can raise falls, injuries, chronic pain, and long-term musculoskeletal utilization for GLP-1 users. Muscle loss often flies under the radar because it is not clearly coded or routinely discussed. For benefits leaders and health plans, that makes it a costly blind spot.
Most anti-obesity medications work by suppressing appetite or altering satiety signals. Whether it's semaglutide (GLP-1), phentermine/topiramate (Qsymia), or bupropion/naltrexone (Contrave), reduced appetite or altered satiety often leads to a meaningful calorie deficit.
That deficit drives weight loss but it doesn’t tell the body to preserve muscle. Unless a member has support that helps preserve lean mass, weight loss may include both fat and muscle. This is especially problematic because most GLP-1 candidates already start out inactive: fewer than 1 in 4 U.S. adults meet the CDC’s recommended activity guidelines.² In other words, the majority of weight loss drug users may be losing strength along with weight and entering a physically deconditioned state.
Lean muscle loss is a dangerous side effect of GLP-1 weight loss drugs
Muscle does more than support movement:
- supports joint integrity and spinal alignment³
- supports metabolism and energy use at rest⁴
- helps reduce fall and injury risk⁵
- helps preserve independence in daily life⁶
When muscle mass declines:
- Balance worsens, fall risk increases⁴
- Joint pain becomes more common as muscles fail to support the skeleton³
- Recovery slows following injury or illness³
- Energy drops, reducing adherence to positive behavior change³
Muscle loss changes the risk profile of a member’s health, even if the scale shows an objectively positive result of weight lost. Employers and health plans need to look beyond the weight-loss number and support treatment plans with structured wraparound care that helps preserve lean mass.
The MSK claims you don’t see coming
Muscle loss doesn’t appear in a line item on your claims dashboard. But its impact is there, just delayed, and disguised. Research links sarcopenia (progressive loss of muscle mass, strength, and function) with:
- up to 33% of chronic pain cases in older adults⁶
- a 60% higher risk of falls⁵
- a 2.5x higher disability risk when combined with obesity⁷
And when members on weight loss drugs lose muscle, the signs don’t show up in weight management metrics. They show up in the months and years after treatment in the form of musculoskeletal issues that require significant (and expensive) medical intervention:
- Joint pain and mobility complaints
- Fall-related injuries and ER visits
- Referrals to orthopaedic specialists
- Slower return-to-work after minor incidents
- Increased pain medication use
Even when short-term weight-loss results look positive, lean-mass loss can quietly become a longer-term musculoskeletal cost driver.
Who’s most at risk of muscle loss during weight loss?
The muscle loss effect isn’t evenly distributed. The following groups are especially vulnerable to sarcopenia:
- Infrequently active members: most GLP-1 users fall into this group
- Adults over 40: natural sarcopenia in middle and older age amplifies the risk
- Desk-based workers: sedentary time increases lean tissue degradation
- Those with chronic MSK pain or injury history: weakened muscles accelerate recurrence
- Women post-menopause: hormonal shifts reduce muscle preservation capacity
These populations often overlap with high-prescription segments meaning muscle loss is a common risk for weight loss patients considering GLP-1 usage. The solution is prevention.
The strategic takeaway is prevention. By building structured support around GLP-1 treatment, plans can help members preserve strength, build healthier routines, and improve the odds that outcomes hold after treatment changes or ends.
Prescribe structured movement alongside GLP-1 weight loss drugs
Advice alone rarely creates durable behavior change at scale. To better protect lean mass during weight loss, plans need structured support that begins early and continues consistently. Movement matters, but so do nutrition guidance, accountability, and long-term habit support.
Movement + medication is part of the GLP-1 prescribing guidance
What we’re suggesting isn’t just good practice, it’s standard protocol. GLP-1 medications like semaglutide are only approved for weight management as an adjunct to a reduced-calorie diet and increased physical activity. That’s not a recommendation. The manufacturers of GLP-1s advise supporting movement programs to retain lean muscle mass.⁶
Yet despite this, many patients start treatment without any structured movement plan, putting them at high risk of lean muscle loss, slower progress, and weight regain. Sword Pulse helps close that gap with continuous support designed to reinforce the behaviors medication alone does not create.
Structured physical activity:
- Preserves lean muscle mass to support metabolism
- Reduces fall and injury risk by strengthening stabilizing muscles
- Builds habits that help members transition successfully after discontinuing medication
Healthcare providers can proactively embed movement into a GLP-1 weight loss care model to prevent the dangerous side effect of lean muscle loss before it becomes a downstream cost driver. That is the gap Pulse is designed to address.

How Pulse helps GLP-1 change habits for good
Pulse, the cardiometabolic pillar of the AI Care Platform, is designed to support people managing blood pressure, blood sugar, cholesterol, weight, and GLP-1 use through continuous lifestyle support.
For people using weight-loss drugs, Pulse is built to address what medication alone does not: lean-mass preservation, strength-building support, nutrition guidance, and the day-to-day habits that help results last.
Pulse combines Phoenix, Sword Health’s AI Care Specialist, with guidance from a Health Specialist and connected devices that bring objective health data into each interaction. Members receive support across movement, blood pressure monitoring, nutrition, and daily activity habits, with guidance that adapts over time to what is actually working for them.
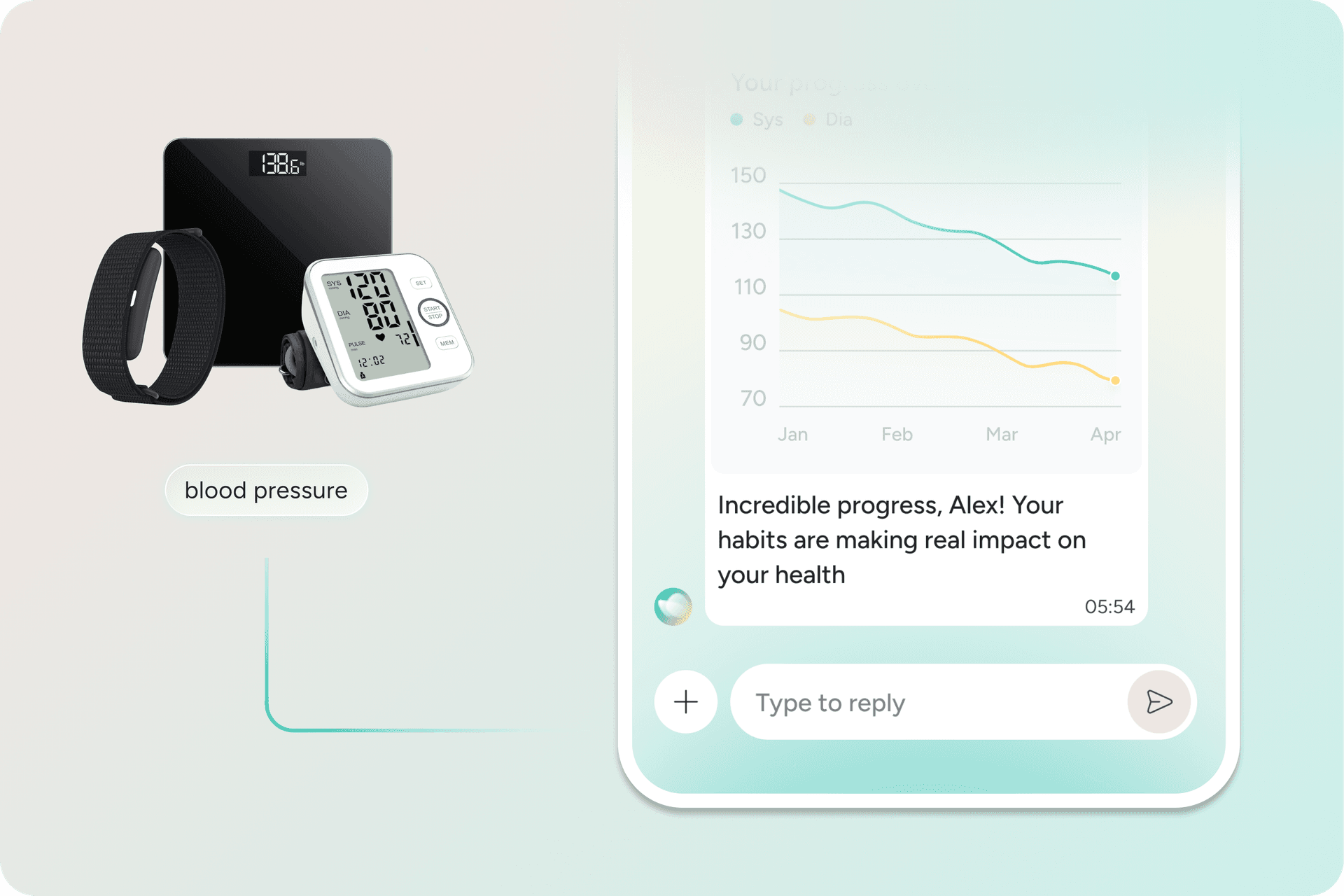
Proven health improvements from Pulse members
Pulse supports GLP-1 users with continuous lifestyle support built around movement, nutrition guidance, and daily habits. In Pulse:
- 83% of members report feeling better or much better¹¹
- 51% of members with low physical activity at baseline reached the World Health Organization recommended activity threshold after 27 days of Pulse sessions¹²
These signals do not prove every downstream financial outcome on their own. But they do show the kind of sustained engagement plans need if they want weight-loss-drug strategies to produce more durable value over time.
GLP-1s initiate change. Pulse makes it last.
GLP-1 medications are not the problem. The medication alone does not cause lean muscle loss. Without structured support, the risk of lean-mass loss and reduced long-term durability becomes harder to manage..
Without movement, members lose muscle, resilience, and long-term value. SPulse provides structured support that helps protect lean mass, reinforce healthier habits, and improve the odds of more sustainable outcomes. If you're offering GLP-1s, Pulse helps you protect your members and drive lasting success.
