Ask a PT: Does walking really help with pain?

If you’ve ever stood on the sidelines of a sporting event, you’ve likely witnessed many falls, trips and tackles. Whether the players are small children or professional athletes, the advice from the coach may have simply been to “walk it off.”
While that is not always the best solution after an acute injury, walking can be a really effective way to manage chronic pain.
Why does walking (and other exercise) help relieve pain?
Motion is lotion. Movement increases blood flow, which brings nutrients to our tissues. It also helps those that don’t have blood flow, like cartilage. Cartilage lines our joints, absorbing impact. It’s surrounded by a liquid which provides it with nutrients, flowing in and out of it like a sponge. Exercise, like walking, causes loading that fills and squeezes that sponge, particularly in the joints of our legs and spine.
Movement of all kinds, including walking, can also make you less sensitive to pain. If you stub your toe before riding your bike, you’ll feel it more than you would if you stubbed it right after getting off your bike.
This happens for several reasons. One is that exercise releases hormones and neurotransmitters. These work to reduce pain and improve our mood - even decreasing symptoms of anxiety and depression. The other is that while we’re moving, we’re concentrating on something else: our breathing, the sounds, the landscape, and making sure not to trip over the cracks in the sidewalk. Of course, your mileage (literally) may vary: the amount of exercise it takes to decrease pain as well as how long the pain-relief halo lasts after exercise varies from person to person and the type, difficulty and duration of exercise you’re doing. But trust the neuroscience - the pain relieving effect of exercise is the real deal.
How to walk your way to pain relief
Walking is a simple, low-impact way to incorporate movement into your life. If you can, head to a local park or track to walk outdoors. Being outside benefits our mood and health. If that won’t work for you, you have other options! You can walk indoors using a treadmill or even walk laps around your home or another building (just make sure to change the direction you’re walking your laps every 10 minutes or so). You don’t need any equipment, but a good pair of closed-toe shoes will help. Make sure they feel comfortable and fit well.
First, check with your doctor about health considerations, such as heart or lung problems that may affect your ability to participate in a walking program. If you have one of these conditions or are experiencing pain that’s causing you to limp or worsens with walking, ask a physical therapist for guidance.
Once you’ve been cleared by your doc, start with a small amount of walking three days per week - try 10-15 minutes. Build the amount of time you’re walking by adding 2-5 minutes per walk until you can do 30 minutes, then add in another day of walking. After a week or two, add a fifth day of walking to your schedule. Here is an example:
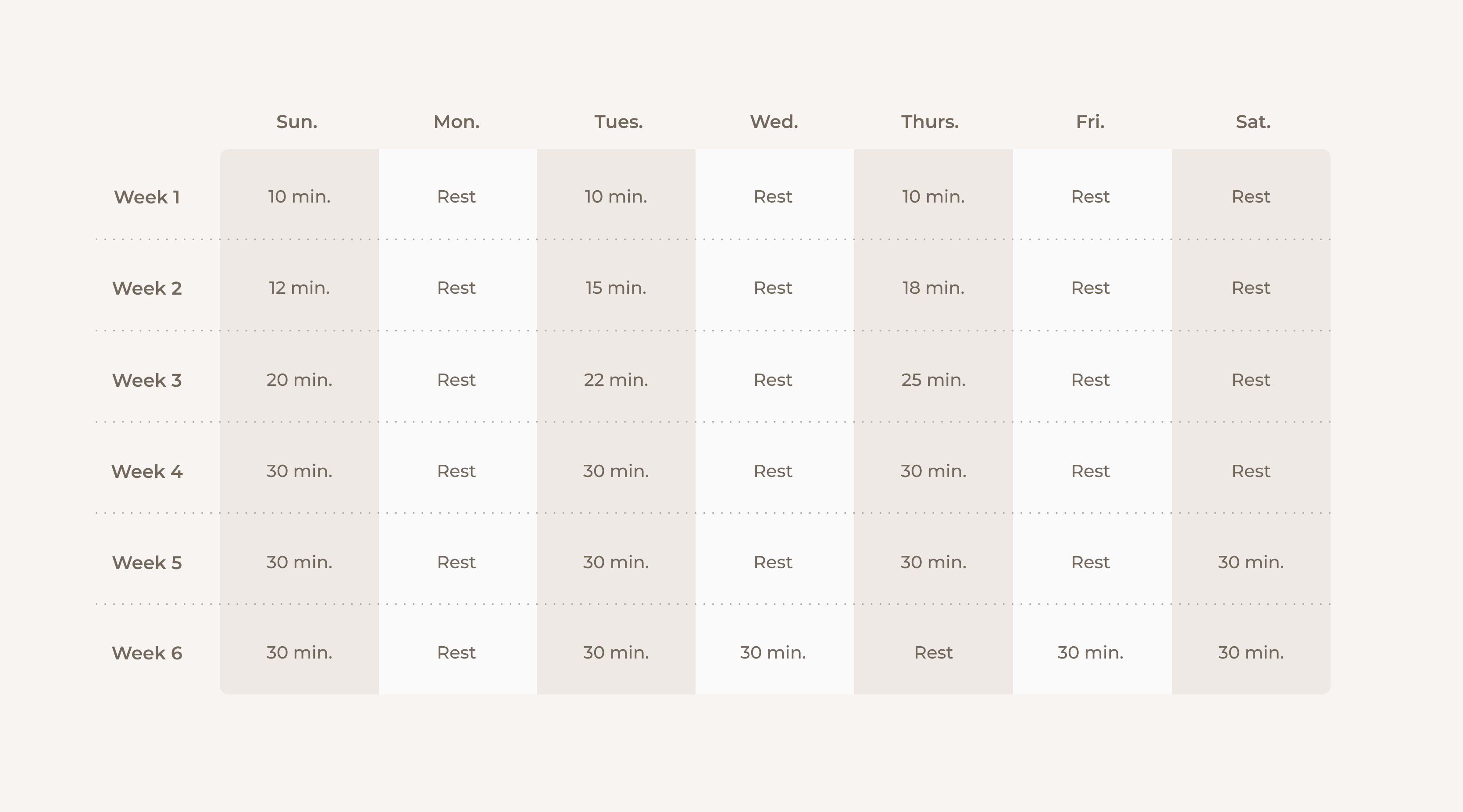
You can always move days around, but try to spread your walking out. It’s more beneficial to walk every other day than to walk three days in a row, then take four days of rest.
Once you are walking for 30 minutes at a time, five times per week, you have a choice. You can stay there - that’s a great amount to make a habit! If you’d like to level up, you can extend the length of your walk, add a sixth day of walking, or mix up the terrain or speed. Walking up and down hills or alternating 1-2 minutes of fast walking with 1-2 minutes of easy walking during your walk makes a 30 minute walk much more challenging.
Remember, consistency is key! And if you don’t enjoy walking, there are many other types of exercise that can help you manage your pain and overall health, including running, cycling, swimming, yoga and strength training. Talk with your physical therapist about your interests. They will help you create a long-term plan you’ll enjoy.
About the author: Megan Hill, PT, DPT
Megan Hill, Doctor of Physical Therapy, is a licensed physical therapist focused on musculoskeletal rehab and chronic pain management. She dropped her plans to go to law school for physical therapy after a knee injury from the Chicago Marathon left her in need of rehab, and she hasn’t looked back since. She’s on a mission to empower people to manage their health through exercise, education and coaching, rather than relying on passive approaches.
Megan earned a Doctor of Physical Therapy degree from the University of Illinois at Chicago (UIC). She also holds a Bachelor of Arts degree in psychology from Duke University and is a certified running coach.
Megan lives in Denver, Colorado, where she spends every spare second running, biking, hiking, sailing and stand up paddleboarding with her husband, Layton, and dog, Ollie.


