What is Pelvic Organ Prolapse?
Pelvic organ prolapse (POP) is a disorder in which the muscles and tissues of the pelvic floor can no longer adequately support the pelvic organs and they drop down or press into the walls of the vaginal canal.1
Three different types of POP are outlined below. These are named based on the pelvic organ that is descending1.
- Cystocele occurs when the bladder drops into the vaginal canal
- Uterine prolapse occurs when the uterus drops into the vagina
- Rectocele occurs when the rectum bulges into the vagina
Pelvic organ prolapse is very common for women over 40
POP prevalence increases as a woman ages. In fact, 74% of women between 40-59 have POP.² However, aging is not the only risk factor for this condition. Other common risk factors include genetics, connective tissue disorders, obesity, pelvic floor injuries, hysterectomies, and hormonal changes associated with menopause and pregnancy.³
Pelvic organ prolapse can also occur following childbirth³ and is particularly seen in women who’ve had multiple vaginal deliveries and/or given birth to a baby weighing more than 8.5 lbs. Habits or activities that cause excessive strain on the pelvic floor can also lead to POP.
Examples include constipation, chronic coughing due to smoking or lung disease, and high-impact exercise or jobs that require heavy lifting.³ Unfortunately, the symptoms impact physical as well as mental health and women with chronic issues can experience significant challenges dealing with the impact of these changes to their day-to-day life.
Symptoms of pelvic organ prolapse
The symptoms of POP can be very debilitating for some people, however, not all individuals who have POP will experience symptoms⁴. In rare circumstances, POP can occur suddenly as a result of significant strain causing the last bit of connective tissue that is supporting the pelvic organ to give way. However in most cases, women begin experiencing a variety of pelvic symptoms that worsen over a period of time, until the actual prolapse is discovered. Symptoms of POP can include⁴:
- Sensation of vaginal bulging or heaviness, like “something is falling out”
- Pelvic pressure, dullness, aching or discomfort that progressively worsens as the day goes on, or with activities that can cause downward strain such as high-impact exercise and/or coughing
- Urinary leakage or inability to fully empty bladder
- Difficulty having bowel movements and fully emptying stool
- Difficulty inserting tampon
- Painful intercourse
- Low back pain

How to confirm a pelvic organ prolapse diagnosis
POP is diagnosed via a pelvic examination performed by an OB/GYN or urogynecologist⁵. To assess the severity of the prolapse, individuals are asked to cough or bear down, which replicates the effect of increased intra-abdominal pressure on the pelvic organs⁵.
The provider will then grade the severity of the prolapse based on how far the organ drops in relation to the vaginal opening. If the prolapsing portion does not drop past the vaginal opening, the prolapse is considered grade 0-2. If the prolapsing portion drops partially3 or completely4 past the vaginal opening, it is considered grade 3-4⁵.
In some cases, it can be difficult to accurately identify which organ is prolapsed. Therefore, some providers will classify the type of POP by the part of the vagina that is prolapsing (front, top, back) and not the actual pelvic organ.
Impact of POP on quality of life
The severity in which POP impacts one’s quality of life (QOL) varies widely. For some women, POP can be a minor frustration that can be managed by avoiding certain activities that may cause symptoms. For those with severe symptoms, POP can greatly impact all areas of their life⁵. Importantly, people dealing with pelvic floor dysfunction of any kind can experience a negative impact on their mental health⁵.
Below are some examples of how POP can impact QOL:
- Negative beliefs about themselves and their bodies
- Pain with intimacy or fear of intimacy
- Avoidance of high impact exercise (ex: heavy weight lifting, jumping, running)
- Physical difficulties with symptom aggravation by occupational duties
Pelvic organ prolapse treatment and recovery options
There are a variety of different care options for people suffering with POP. Surgery is one option⁵, but often there are less invasive alternatives to consider. Here are four of the most common:
1. Surgical intervention
Surgical intervention can include using body tissue or synthetic mesh to repair the prolapse and provide pelvic support for the organs. Research indicates that by age 79, women have an 11% chance⁷ of undergoing at least one surgery for POP or incontinence, with this risk potentially doubling in the next 30 years due to an aging population. Unfortunately, the long-term outcomes of POP surgery are not favorable. After 5 years, 41% of women who underwent surgery for POP experience recurrence and 10% required another surgery.
2. Pessary usage
A pessary is a removable device that is inserted into the vagina to provide support to the vaginal walls and pelvic organs. Pessaries are a non-invasive treatment option that may help reduce the symptoms of POP and urinary incontinence. They are often used in conjunction with other treatment options including weight management and pelvic floor strengthening to maximize symptom relief.
3. Obesity management and diet
Since excess weight within the abdomen causes added pressure on pelvic organs and the pelvic floor, maintaining a healthy weight may prevent POP from occurring. For individuals with POP who are overweight, weight loss³ is a recommended treatment option. Typically this involves a combination of exercise and dieting. Individuals are also encouraged to eat a high-fiber diet to prevent constipation and the need to strain with bowel movements.
4. Pelvic floor therapy
Pelvic therapy is another non-invasive option⁸ to address the symptoms of POP. Pelvic therapy can not only reduce the severity of symptoms in those already suffering from POP, but also may help decrease the development of POP. Pelvic-floor therapy often includes a combination of the following:
- Exercises to strengthen the pelvic and abdominal muscles for increased support of pelvic organs.
- Activity modification to reduce the amount of pressure placed on pelvic organs.
- Bladder/bowel training to promote healthy habits around toileting.
Sword Bloom: pelvic health care you can use at home
Bloom offers personalized care programs for individuals suffering from POP that are accessible from home with 24/7 support from a Women's Health Specialist that has a Doctor of Physical Therapy degree. Each program is prepared by the member's matched specialist based on their health history and specific symptoms using a variety of techniques including strengthening exercises, activity modifications, and bladder/bowel training.
How does Bloom work to help manage and reduce pelvic pain?
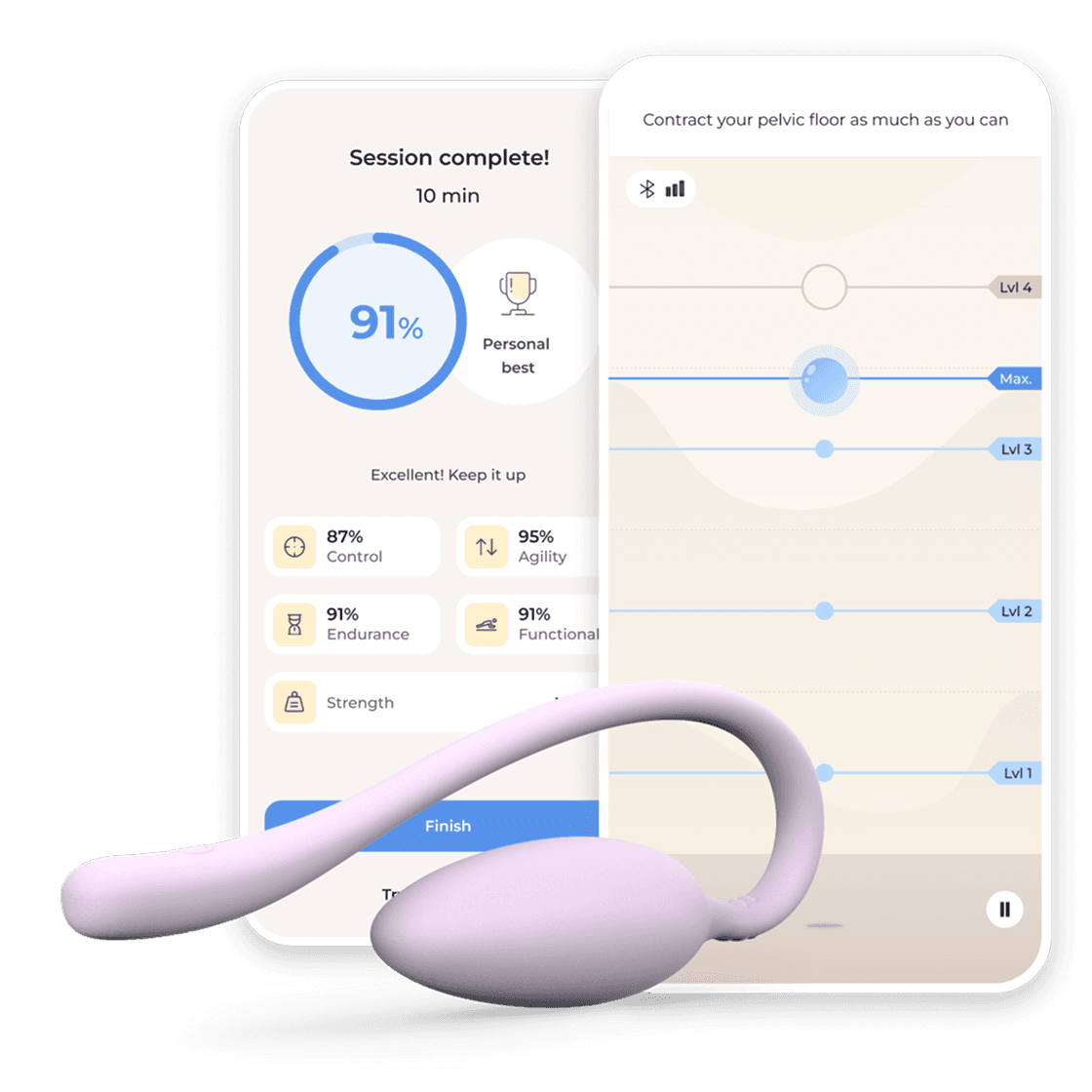
Bloom helps women strengthen their pelvic-floor and abdominal muscles through a customized exercise program, guided by their Women's Health Specialist. Members receive the Bloom Pod, an FDA-listed device⁹ that measures pelvic floor muscle activity. Using the Sword app, women complete short, guided sessions at home. The Pod provides real-time biofeedback, allowing users to see and understand how their muscles are working.
Throughout treatment, the specialist monitors progress, adjusts exercises, and provides education and encouragement through secure messaging or video calls. The experience mirrors in-person therapy but is more accessible and private.
Why pelvic floor dysfunction treatment at home is so much easier
Despite its proven benefits, pelvic floor therapy can be difficult to access. In the U.S., there is only one pelvic health therapist for every 10,000 women¹² leaving long wait times and significant travel burdens. Privacy concerns and busy schedules add further barriers, especially for mothers and caregivers.
Bloom's from-home women's health programs make pelvic care more accessible, flexible, and discreet. Women can complete guided sessions at home, supported remotely by licensed pelvic health specialists. This empowers women to take control of their recovery at their own speed, combining comfort and consistency with clinical precision.
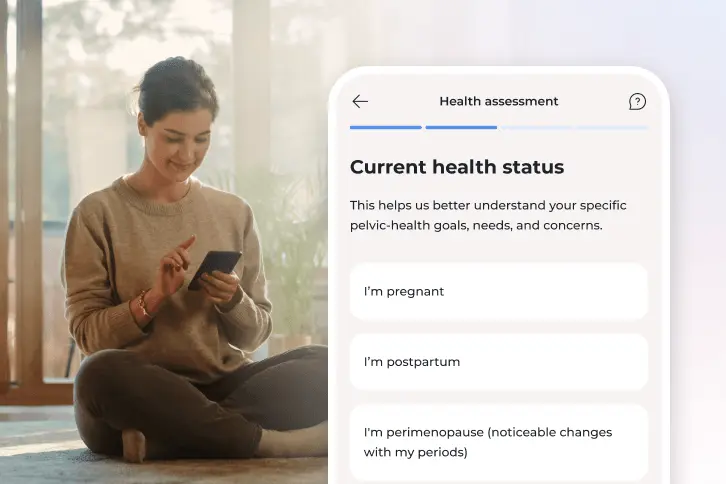
What to expect from Bloom
How Bloom supports you, step by step
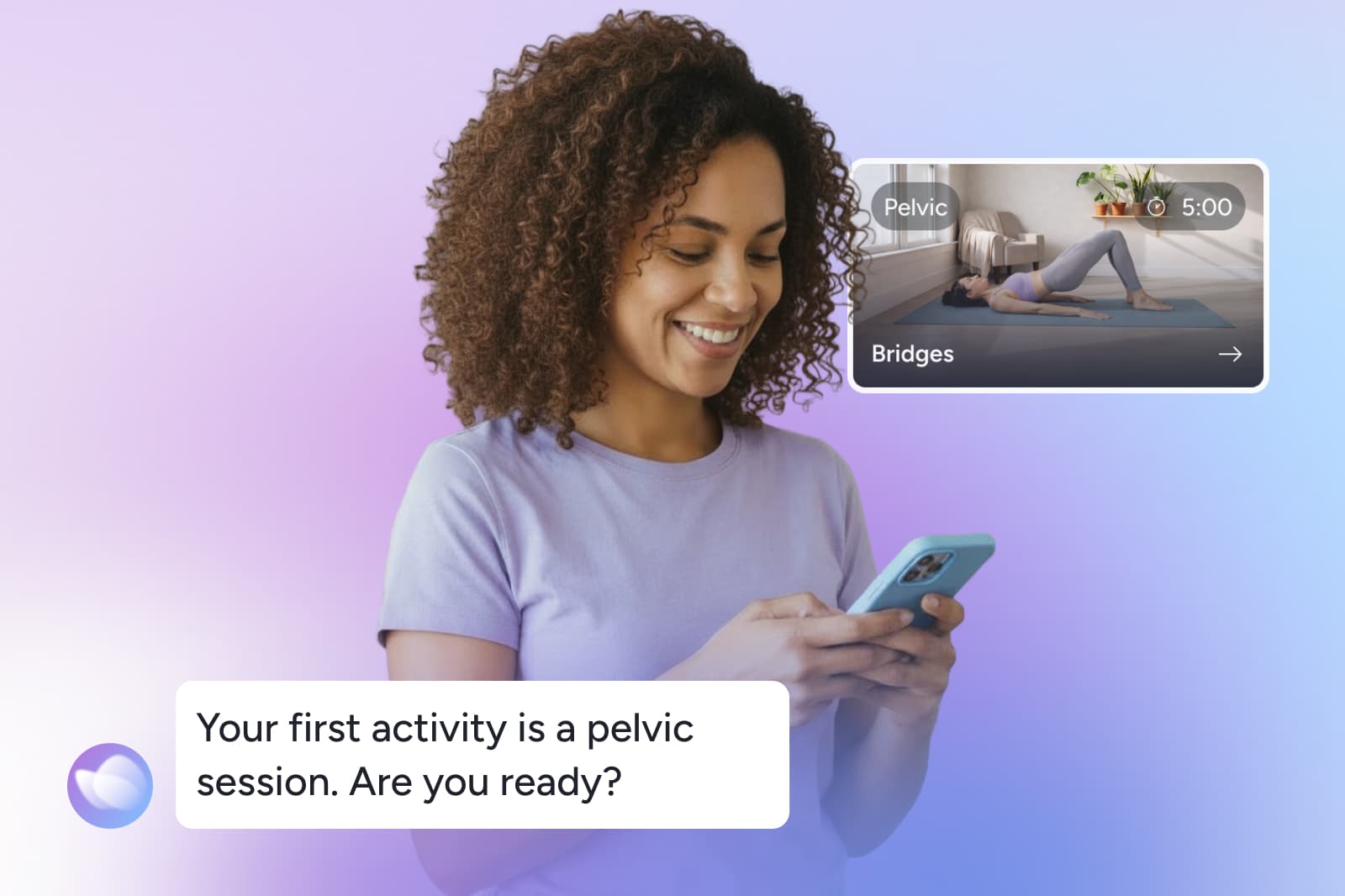
1. Tell us what you’re experiencing
Share your symptoms, goals, and what you need support with so Bloom can tailor your plan.

2. Meet your Women’s Health Specialist
Match with a Women’s Health Specialist who holds a Doctor of Physical Therapy degree and helps guide your plan.
3. Receive your Bloom kit
We’ll send everything you need, including the Bloom Pod, directly to your door.
4. Start guided sessions from home
Use Bloom privately from home with real-time feedback and 24/7 support along the way.
Why Bloom is so effective compared to alternatives
Bloom combines clinical rigor with real-world flexibility. Traditional therapy often requires weeks of travel, time off work, and out-of-pocket costs. Bloom removes those barriers while maintaining medical-grade supervision. Clinical outcomes show Bloom's strong results⁹:
- 61% of women with moderate-to-severe pelvic floor dysfunction experienced meaningful improvement.
- 76% reported reduced anxiety, and 54% saw improvement in depression symptoms.
- Productivity impairment decreased by nearly 50%.
- Half of all sessions take place outside normal working hours, and 20% occur on weekends.
Bloom’s combination of privacy, flexibility, and professional oversight makes it one of the most accessible and effective pelvic care options available.
Take back control of your body with private, discreet from-home care
If you are dealing with pelvic discomfort, pain, or leakage, you do not have to manage it alone. Pelvic therapy can help you rebuild strength, control, and comfort, and with Bloom, you can do it discreetly and effectively from home. Recovery is guided by one-on-one clinical guidance from a Women’s Health Specialist holding a Doctor of Physical Therapy degree. Bloom's care programs are supported by real data, and designed for your life and schedule. It is care that meets you where you are, helping you move forward with confidence.
Are you already covered for Bloom's personalized care programs by your employer or health insurer? Check your coverage today (you may be able to get started today at $0 cost to you).
While we use the word "women" in some of our communications, Bloom is designed for all individuals with vaginal anatomy regardless of gender identity. This article is intended for educational purposes only, using publicly available information. It is not medical advice nor should it be used for the diagnosis, treatment, or prevention of disease. Please seek the advice of your physician or another licensed medical provider for any health questions or concerns. In case of emergency, call 911.

