The Sword Summary Warm-up
Don’t have time for the full workout? We’ve got you covered with a quick, high-intensity session. Here are the key takeaways:
- Menopause joint pain is common and often linked to hormonal, muscular, and pelvic changes¹
- Joint discomfort may be influenced by how your body stabilizes and supports movement, not just the joints themselves
- Personalized women’s health support can help you better understand and manage these changes from home
Why joint pain can show up during menopause

Joint pain during menopause can feel unexpected. You might notice stiffness in your knees when getting up, aching hips after sitting, or discomfort in your hands that was not there before.
For many women, these sensations seem to appear without a clear cause. That can make them harder to trust or understand. You may find yourself wondering if something is wrong, or if this is simply something you have to live with.
Menopause brings real physical changes. These changes can affect how your joints feel, how your muscles respond, and how your body moves as a whole. When you understand why these changes happen, it becomes easier to respond in a way that supports your body instead of working against it.
Joint pain during menopause rarely has a single explanation. Instead, it often reflects a combination of changes happening at the same time.
Hormonal changes can affect your joints during menopause
Estrogen plays an important role in maintaining joint health. As estrogen levels decline during menopause, tissues around the joints may become less flexible and less well-lubricated. This can lead to:
- Increased stiffness, especially in the morning
- Reduced range of motion
- A feeling of tightness during movement
What this means for you is simple. Your joints may feel different even if your activity level has not changed. Pain and discomfort can often develop. But you can also often manage, minimize, and prevent these symptoms.
5 ways to prevent joint pain in menopause
This stage of life often brings new sensations, but your body is still capable of strength and adaptability.
The decline in estrogen during menopause affects the entire musculoskeletal system. This hormone influences collagen production, inflammation, and the body’s ability to repair tissue. When estrogen levels fall, joints may lose some of their elasticity, and recovery after exertion can take longer⁹.
These changes are not permanent. They are part of the body’s process of adjusting to a new balance. Your joints can stay mobile for decades to come with steady care, movement, nourishment, and guided support.
First, learn how menopause can impact your joints
Menopause affects every part of your body’s movement system. When estrogen levels drop, your body produces less collagen, the protein that gives structure and elasticity to cartilage, tendons, and ligaments⁴. Estrogen also helps maintain joint lubrication, keeping movements smooth and pain-free.
As this hormone declines, the tissues that surround your joints can lose hydration, and the fluid that cushions your knees, hips, and shoulders becomes less abundant⁵. Over time, this can make your joints feel stiff or creaky, especially after periods of sitting or when you first wake up. Without regular motion, that stiffness can build up, making movement feel more effortful and less natural.
It is important to remember that this change is not permanent or harmful. It is your body’s way of adjusting to a new hormonal rhythm, and movement is key to helping it adapt.
Next, we will explore how to manage joint pain effectively and why each step matters.
1. Keep moving to improve your joint health
Gentle, consistent movement keeps your joints nourished and flexible. When you move, you increase circulation, deliver nutrients to tissues, and help your body produce more synovial fluid, the natural lubricant that protects your joints⁶.
This is not about intense workouts or pushing through pain. It is about showing your body that movement is safe and beneficial.
- Move a little, often. Aim for 30 minutes of light activity most days. Walking, swimming, cycling, or yoga are gentle ways to improve mobility and reduce inflammation⁷.
- Add small bursts of movement into your day. Try standing every hour, rotating your wrists, or rolling your shoulders while waiting for the kettle to boil.
- Stretch after sitting. Hip circles, knee bends, and gentle spinal twists release tension that builds during long periods of stillness.
- Start slow if you have been inactive. Even a five-minute walk after meals can improve circulation and reduce stiffness.
Movement reminds your body that it is adaptable and strong. Each step helps rebuild comfort, stability, and confidence.
2. Strengthen your core and pelvic alignment
Your pelvis forms the foundation for posture and movement. During menopause, hormonal changes can affect the muscles that stabilize your pelvis and core. These muscles may become tighter or weaker, altering your balance and placing more strain on the hips and lower back¹⁷.
This imbalance can make everyday tasks like walking, bending, or sitting feel slightly less stable. Supporting pelvic and core alignment improves posture and reduces joint stress.
How you can strengthen your core and improve alignment
Strengthening your core and pelvic muscles helps your whole body move more efficiently.
- Breathe with awareness. Deep breathing activates your diaphragm and deep core muscles that stabilize your posture.
- Add simple core exercises. Bridges, bird-dog, and side-lying leg lifts build coordination and support.
- Avoid straining. Exhale as you lift, reach, or bend to protect your spine and pelvic floor.
- Check posture throughout the day. Keep your shoulders relaxed and your core lightly engaged.
Programs like Bloom provide guided pelvic care tailored to your needs, helping you strengthen safely and consistently. Bloom is a digital women’s health solution designed to help women manage perimenopausal symptoms like joint stiffness, back discomfort, and pelvic tension.
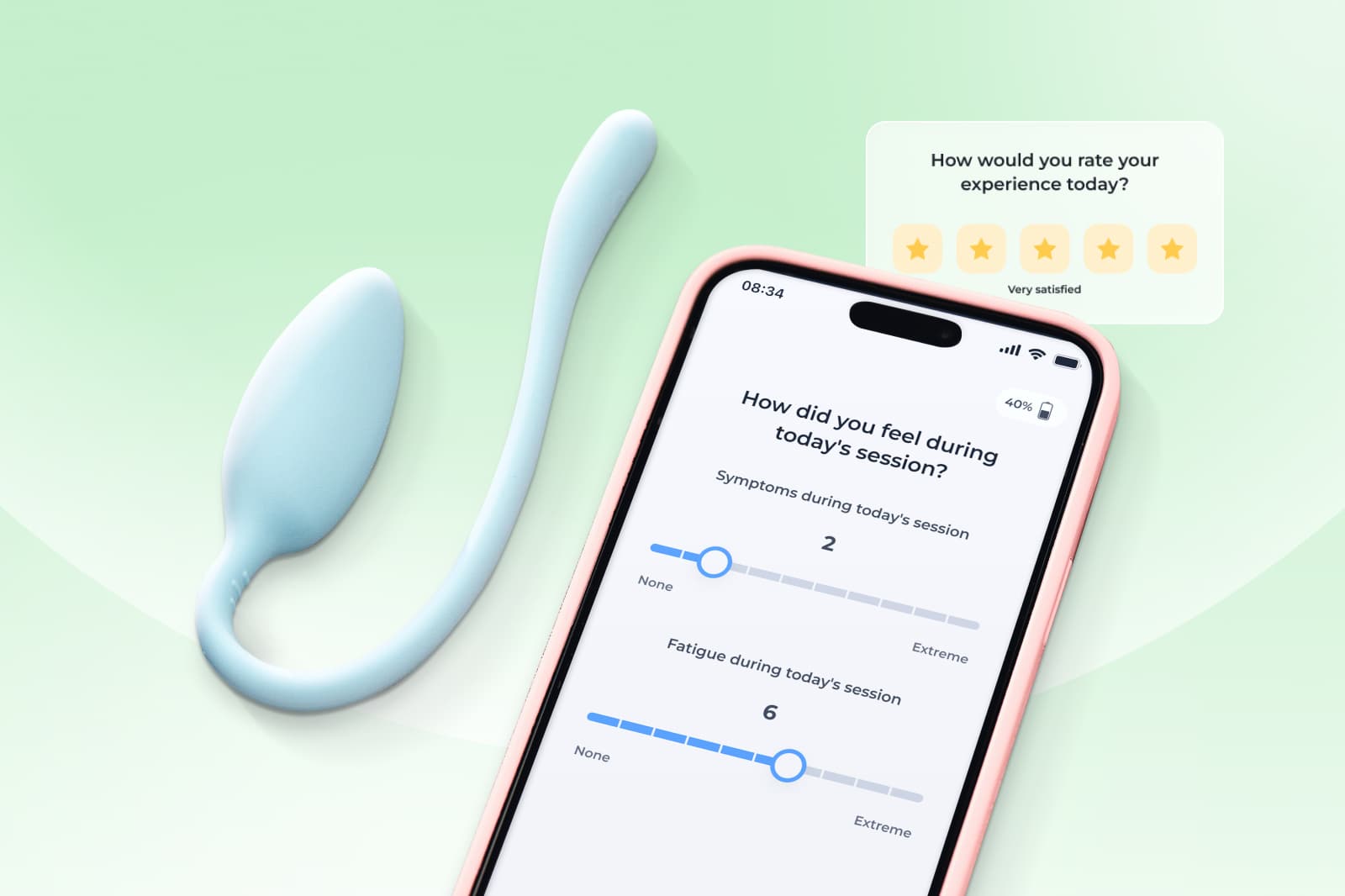
Each member is paired with a Women’s Health Specialist (Doctor of Physical Therapy) who creates a personalized care plan focused on strength, posture, and mobility. Members access short, guided sessions through the Sword Health app and use the Bloom Pod which is a safe, FDA-listed biofeedback device that provides real-time feedback during exercises.
3. Manage inflammation after exercise
Hormonal changes influence how your body manages inflammation. Estrogen helps regulate immune activity and antioxidant balance. When levels drop, inflammation can rise more easily, especially in the joints and connective tissues¹¹.
This means your body may feel more sensitive after exercise or during stressful weeks. You might notice stiffness that lingers longer than before, or a general feeling of heaviness in your limbs. Lifestyle factors such as sleep and nutrition can amplify or reduce these sensations.
This inflammation is not harmful in itself. It is your body’s way of adjusting to new hormonal patterns. With the right support, your system can rebalance.
How you can calm inflammation and support recovery
Your diet and hydration influence how your joints feel and heal. Choosing anti-inflammatory foods and prioritizing hydration can help reduce soreness and support repair.
- Include omega-3s often. Foods like salmon, flaxseed, and walnuts reduce inflammation and protect joint tissue¹².
- Eat colorful foods. Berries, spinach, and peppers supply antioxidants that fight oxidative stress.
- Stay hydrated. Water supports joint lubrication and helps remove metabolic waste¹³.
- Limit highly processed foods and excess sugar, which can increase inflammation.
If meeting nutritional needs through food alone is difficult, discuss supplements such as vitamin D, magnesium, or omega-3s with your clinician.
4. Restore muscles by prioritizing flexibility and rest
Many women notice their muscles feeling tighter or less responsive during menopause. Estrogen affects not only the joints but also muscle tone throughout the body. When hormone levels drop, muscles can lose elasticity, especially around the hips, shoulders, and back¹⁴.
Sleep can also become disrupted, slowing recovery. When you do not sleep well, your body produces more cortisol, a stress hormone that increases inflammation and pain sensitivity¹⁵. Over time, this can create a cycle of stiffness and fatigue.
You can interrupt this cycle with a few restorative habits that improve both rest and flexibility.
How you can improve flexibility and get better rest
A combination of gentle stretching and good sleep hygiene helps your body relax, repair, and restore strength.
- Stretch before bed. Spend a few minutes loosening your hips, shoulders, and back while breathing deeply.
- Create a calming routine. Reduce screen time and lower lights before bed to signal your body it is time to rest.
- Practice mindful breathing during movement. Inhale through your nose and exhale through your mouth to release tension.
- Keep consistent sleep times. Going to bed and waking up at the same time each day supports hormonal balance and tissue recovery¹⁶.
Better rest supports better movement. You will likely notice less morning stiffness and improved energy.
5. Prevent pain by building muscle strength
During menopause, changes in estrogen levels affect more than flexibility. Estrogen helps maintain lean muscle mass and bone density. As levels decline, your body naturally loses some of that strength and stability, which can increase the workload on your joints⁸.
When muscles around the joints weaken, those joints bear more pressure. Over time, this can lead to fatigue, stiffness, and slower recovery after activity.
This loss of strength is not permanent. Muscles respond quickly to consistent, gentle training. Building strength protects your joints and restores energy to daily movement.
How Bloom supports women through menopause
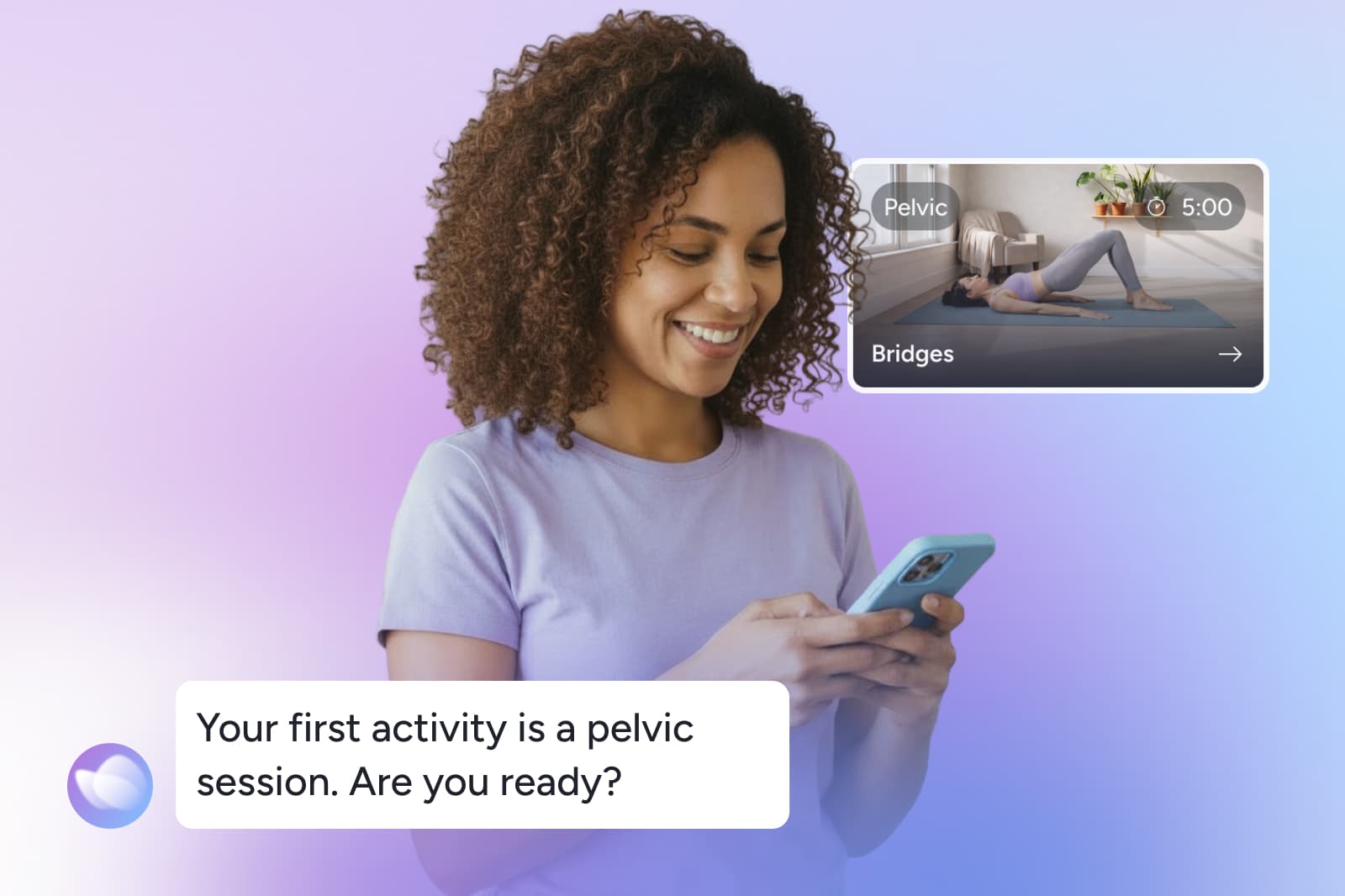
If you are trying to understand and manage menopause body aches, you do not have to do it alone. Bloom is specifically designed to relieve women's health symptoms from the comfort of home. Bloom supports women in every life stage, with dedicated programs for women in menopause.
Members get their own personalized care program care with 24/7 access to expert support, guided by a Women’s Health Specialist that holds a Doctor of Physical Therapy degree. Your plan is tailored to your symptoms, your goals, and how your body responds over time. With Bloom, you can:
- Follow a personalized program designed for your needs
- Receive one-on-one guidance and adjustments as you progress
- Access support privately, from home, on your schedule
- Build confidence in how your body moves and feels
For women navigating menopause, Bloom can support symptoms related to pelvic and core changes, including bladder or bowel changes, pelvic discomfort, and coordination challenges that may contribute to overall body aches. Bloom also integrates technology that helps you better understand how your body is responding during sessions, so your program continues to evolve with you. Importantly, Bloom does not diagnose medical conditions. Instead, it provides supportive, personalized care that helps you better understand and manage what you are feeling.
What to expect from Bloom
How Bloom supports you, step by step
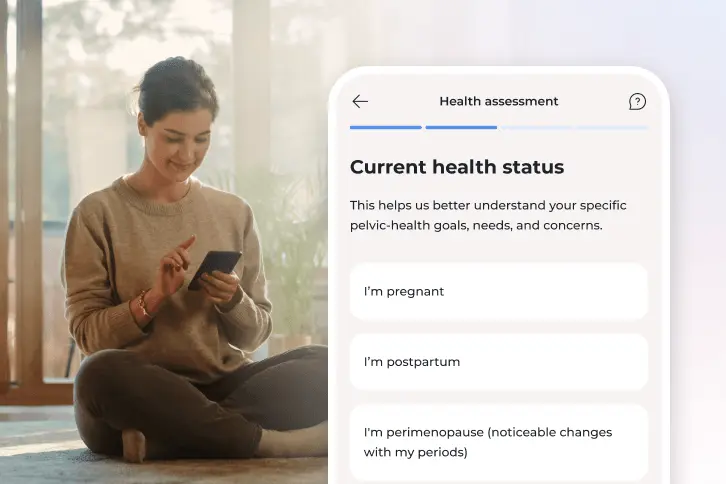
1. Tell us what you’re experiencing
Share your symptoms, goals, and what you need support with so Bloom can tailor your plan.

2. Meet your Women’s Health Specialist
Match with a Women’s Health Specialist who holds a Doctor of Physical Therapy degree and helps guide your plan.
3. Receive your Bloom kit
We’ll send everything you need, including the Bloom Pod, directly to your door.
4. Start guided sessions from home
Use Bloom privately from home with real-time feedback and 24/7 support along the way.
What results can feel like over time
As women build awareness and follow a personalized plan, changes often go beyond physical sensations. In Bloom’s menopause-focused population:
- 65% of women reported improvements in how symptoms affected their daily life
- 56% saw improvements in productivity and daily functioning
- 67% reduced their intention to seek additional interventions
These outcomes reflect something important. When women feel supported and understand their bodies better, they often feel more in control.
Take the next step toward moving with confidence
Menopause joint pain can feel unpredictable, especially when it shows up without a clear explanation. But these changes are not random, and they are not something you have to ignore.
When you understand how hormonal shifts, muscle changes, and pelvic support all interact, your experience starts to make more sense. And when things make sense, your next steps feel more manageable.
You can begin with small changes, pay attention to how your body responds, and explore support that is designed specifically for this stage of life.
Check your coverage today to see if Bloom is available to you and take the first step toward lasting progress.
