If menopause has made your body feel less predictable, you are probably not imagining it. The changes can creep in quietly, then show up in the most inconvenient moments. You cough and leak a little urine. You feel a strong, sudden need to use the bathroom while driving home on the drive home. Sex feels different, or uncomfortable. Constipation becomes a recurring theme. By late afternoon, you feel "heaviness or pressure sensations" in a way you did not used to.
A lot of women assume this is just how it goes now. But menopause is not a finish line where pelvic health stops mattering. For many women or people with vaginal anatomy, it is the moment when pelvic floor support is so important.
The Sword Summary Warm-up
Don’t have time for the full article workout? We’ve got you covered with a quick, high-intensity summary session:
- Menopause can make pelvic and urinary symptoms more noticeable, including vaginal dryness, urinary urgency, leakage, and discomfort with sex. These symptoms are often grouped under genitourinary syndrome of menopause (GSM).¹
- Evidence shows that pelvic floor muscle training, taught as a structured plan, may improve urinary incontinence outcomes for many women
- Pelvic floor health care in menopause is often more than just kegels exercises. Bloom is an ideal alternative to pelvic floor therapy, offering personalized AI Care plans that include breathing and coordination work, guided habit changes, and the support of women's health specialists all accessible from the comfort of your home ² ³
Menopause can change how your pelvic floor feels
Your pelvic floor is a group of muscles and tissues that supports pelvic organs and helps control bladder and bowel function. It also contributes to sexual function.⁷ During and after menopause, hormonal changes can affect tissues of the vagina and lower urinary tract. Many women experience GSM symptoms such as dryness, irritation, burning, urinary urgency, and discomfort with sex.¹
Menopause is rarely the only factor. Your pelvic floor also carries the history of your life, including pregnancy, delivery, surgeries, heavy lifting, chronic constipation, coughing, and years of breath holding through stress. That mix is why pelvic symptoms can appear for the first time in menopause, or shift in a way that makes old coping strategies stop working.
What can you expect from a menopause pelvic health plan?
A lot of people hear “pelvic floor therapy” and picture one thing: Kegels.
That is only one tool, and it is not the right starting point for everyone. Pelvic floor muscle training can focus on strength, endurance, relaxation, coordination, or a combination, depending on what your symptoms suggest.²
A supportive pelvic care plan often includes several elements working together. The best providers consider your symptoms as one holistic puzzle to solve. Pelvic pain and discomfort is often mentally taxing, and it can impact your broader physical health as your movement is affected. Women's health programs like Bloom are the gold standard, with specialist care for women in perimenopause, menopause, and postmenopause.
Education that makes symptoms feel less mysterious
Before making changes, it helps to understand what’s happening in your body. Pelvic care often begins by identifying any patterns in your symptoms. Your care specialist will help you start to notice when urgency occurs, whether leaking happens with exertion, or if pelvic heaviness increases after prolonged standing.¹ ⁷
Find your pattern instead of forcing a generic plan
Some people’s pelvic floors need more strength. Others are tense and overactive, and may benefit from down-training, learning to better relax the muscles, and improve timing of contraction. Many people sit in the middle, where the inability to properly coordinate the muscles may be the main issue. Doing the wrong thing consistently can make you feel like nothing works, when the real issue is that the plan does not match your body.
Exercises that progress instead of overwhelm
If your plan includes pelvic floor muscle training, it typically involves a structured program with consistency over time. Evidence reviews suggest pelvic floor muscle training can be associated with improved urinary incontinence symptoms compared with no treatment. Many programs are structured over multiple weeks, as consistent practice over time supports meaningful improvement.³
Breathing and pressure management
Your pelvic floor works as part of a broader system that includes your diaphragm (the main muscle of breathing) and the deep core and deep core. Learning how to breathe and activate your deep core without bearing down can make day-to-day movement feel easier and more controlled.⁷
Bladder and bowel habits that reduce symptom loops
Practical habit changes matter because urgency and constipation can influence pelvic symptoms over time. This can include hydration and timing strategies, techniques to calm urgency, and bowel routines that reduce straining, like: ³ ⁷
- Staying adequately hydrated while noticing whether certain beverages (like caffeine, alcohol, carbonation, or acidic drinks) seem to worsen bladder symptoms for you.
- Timing strategies may involve allowing the bladder to fill comfortably rather than urinating “just in case,” which can sometimes increase urgency sensitivity over time.
- Urge-calming techniques, such as controlled breathing or distraction strategies, may help reduce the intensity of sudden urges.
- Bowel routines that may reduce straining such as elevating your feet on a small stool during a bowel movement to support a more natural position
How Bloom can help to reduce pelvic pain in menopause
Many women reach menopause already carrying a quiet mental list of symptoms they have learned to manage around: the intense urge to urinate on the commute, pressure or heaviness in their pelvic region that worsens as the day progresses, discomfort that changes intimacy, constipation that comes and goes, sleep disruption that makes everything harder.
Then they run into the most common barrier of all. Even when they want support, in-person appointments can be hard to access consistently. It is not just the time. It is the scheduling. It is the commute. It is the privacy factor. It is the reality that pelvic symptoms are still something many women hesitate to bring up.
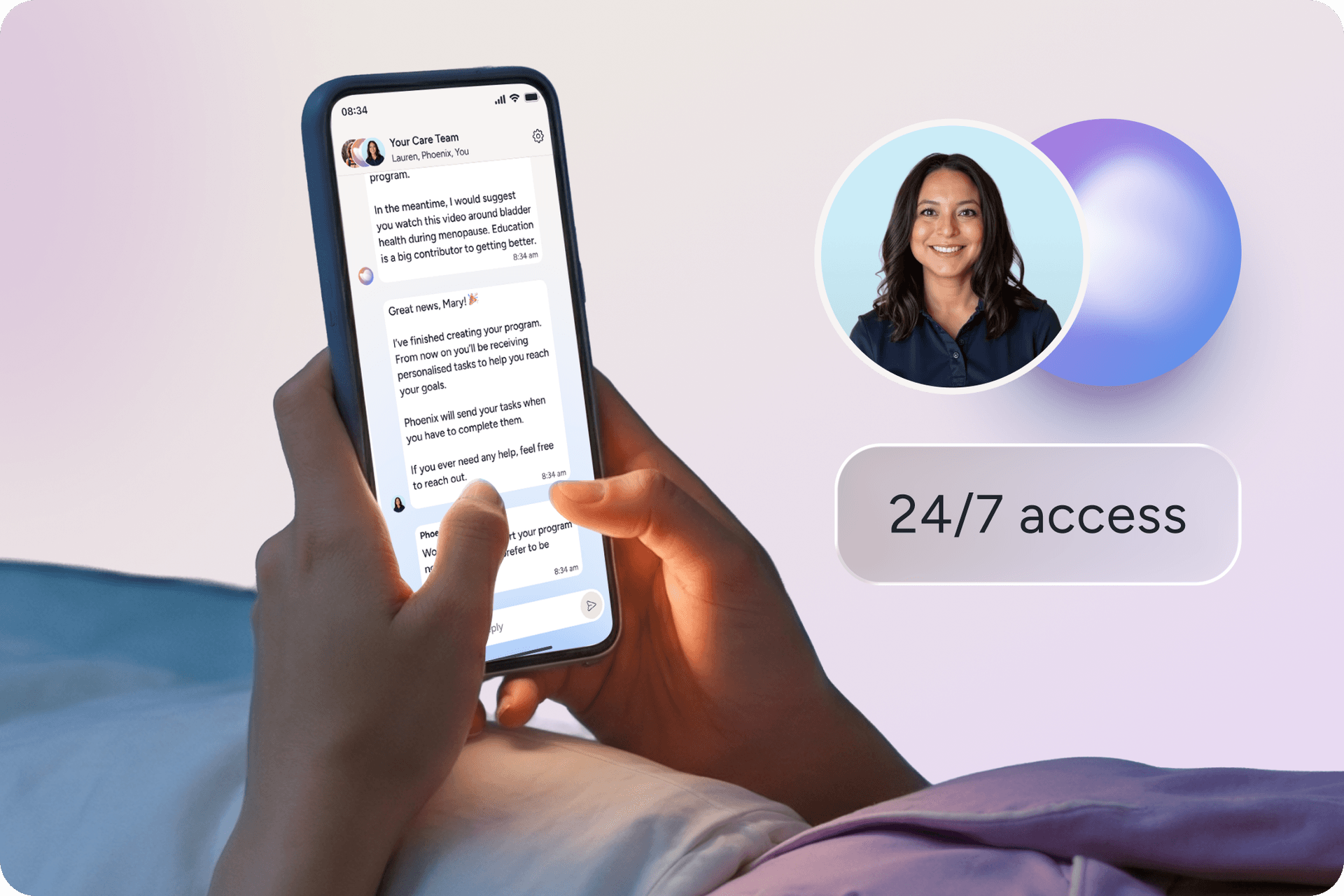
Bloom is a digital women’s health program purpose-built to help meet women where they are, on their schedules, and in private — rather than requiring the “perfect time” to start.⁵ All you need is the Sword app and you have access to a personalized care plan that you can access from anywhere, at any time of the day or night. You also get one-on-one clinical guidance from a Women’s Health Specialist who holds a Doctor of Physical Therapy degree.
What to expect from Bloom
How Bloom supports you, step by step
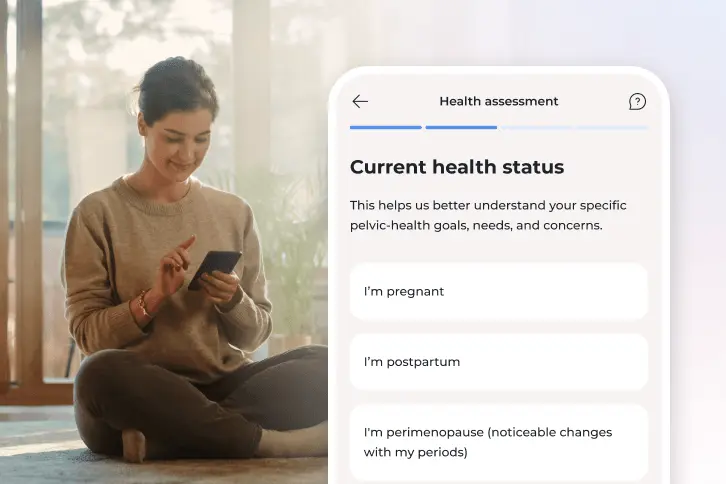
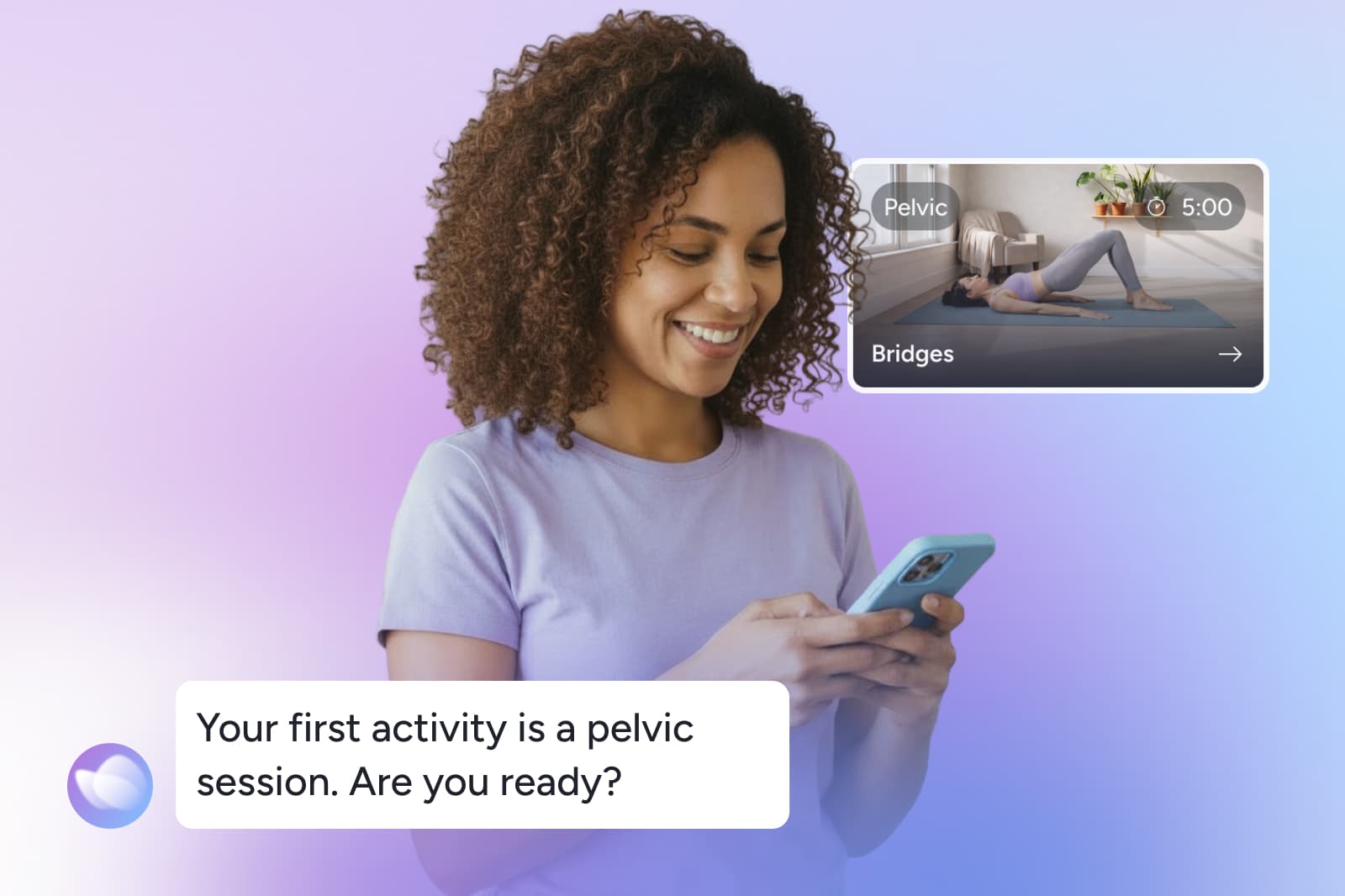
1. Tell us what you’re experiencing
Share your symptoms, goals, and what you need support with so Bloom can tailor your plan.

2. Meet your Women’s Health Specialist
Match with a Women’s Health Specialist who holds a Doctor of Physical Therapy degree and helps guide your plan.
3. Receive your Bloom kit
We’ll send everything you need, including the Bloom Pod, directly to your door.
4. Start guided sessions from home
Use Bloom privately from home with real-time feedback and 24/7 support along the way.
Bloom helps you move from vague advice to clear next steps. Instead of guessing whether you should focus on strengthening, relaxation, coordination work, or habit changes first, you get a personalized plan based on your symptoms and health goals.
Your dedicated women’s health specialist works with you over time, adjusting your plan as your body changes through menopause and postmenopause.⁵
What to expect with Bloom in your first week
When you start with Bloom, the goal is not to hand you a long routine and hope you can stick with it. The goal is to help you understand your symptoms, learn what “right” feels like in your body, and build a plan you can actually follow.
A clearer picture of what your symptoms are signaling: Early on, Bloom helps you identify patterns that often show up during perimenopause, menopause, and postmenopause, including bladder urgency, leaks with exertion, pelvic pressure, constipation and straining cycles, and discomfort that changes intimacy.⁵ Menopause symptoms can feel scattered. Your dedicated women’s health specialist creates a personalized plan and helps connect the dots, so you’re not left relying on guesswork.
A plan that is more than exercises: Many women assume pelvic support is just Kegels exercises or pelvic floor contractions. With Bloom, your personalized care plan may include pelvic floor muscle contractions, but it can also include breathing and pressure management, relaxation and coordination work, and practical habit adjustments that reduce and prevent future symptoms.² ³
Small steps that build confidence: Most women do not need intensity. They need consistency and reassurance that they are doing the right things in the right order. Bloom is designed to fit into your real life so progress can be built without adding a new burden to your schedule. You can complete your set of exercises within 10-15 minutes at any time of the day or night. All you need is the Sword app and your Bloom Pod and you’re all set to go (you can even work on a program without the Bloom Pod is the insertable device is not the right choice for your situation). ⁵
Guardrails for when symptoms need medical evaluation: Bloom is designed to provide support, guidance, and progression. It is not a substitute for urgent or acute medical evaluation. If you report symptoms that could require in-person medical assessment, your Women’s Health Specialist can help you recognize those red flags and guide you to seek evaluation with an appropriate clinician.⁵
When to seek medical evaluation sooner for pelvic symptoms
Pelvic support can be a meaningful step, but some symptoms should be evaluated promptly. Seek medical care if you experience any of the following serious symptoms:
- Bleeding after menopause⁴
- New onset of severe pelvic pain, fever, or feeling unwell
- Sudden inability to urinate or pass stool
- A rapidly worsening bulge sensation or severe pelvic pressure
If you are unsure, it is appropriate to start with a clinician. If you are using Bloom and these symptoms arise, your Women’s Health Specialist can help you recognize when it is time to seek in-person evaluation.⁵
Get expert support and don't accept pain during menopause
If you are not sure whether your symptoms “count,” here is a simple threshold.
If you are changing your life to accommodate symptoms, it is worth exploring pelvic care to get back to the best version of yourself. That is true whether you are in perimenopause, menopause, or years past your last period. You are working through a time of transition and you deserve support that helps you continue showing up in your life, not stepping back from it.
Understanding the broader picture of pelvic health can help explain why these symptoms often show up together. From there, you can focus on what matters most: building a plan that fits your body and your life.
Check to see if your health plan covers Bloom at no cost to you
Many employers and health plans offer Bloom as a covered health benefit. Checking eligibility takes less than two minutes. If you are covered, you can begin your personalized program within days. Check your eligibility now to confirm your access and take the first step from home, on your schedule.

