Tirzepatide and muscle loss: the hidden health plan cost driver
Tirzepatide has quickly become one of the most powerful tools in employer-sponsored weight management. Originally approved for type 2 diabetes and now widely used for chronic weight loss, it helps people reduce appetite and lose weight at a pace that was difficult to achieve in the past. As coverage expands, health plans and employers are seeing strong early engagement and visible results.
But as utilization grows, another significant risk is emerging that health plan leaders need to address. Along with fat, people taking tirzepatide may also lose meaningful lean mass. That is not just a clinical side effect. It can become a cost driver that weakens long-term outcomes, raises musculoskeletal risk, and erodes the long-term value of GLP-1 and GIP/GLP-1 investments. For plans focused on sustainability, better MSK outcomes, and stronger ROI, muscle loss is critical signal.
Why tirzepatide creates downstream risk, not just short-term success
One of the largest studies of tirzepatide followed people using the medication for weight loss for more than a year. The results confirmed what many plans are now seeing in practice. Participants lost a significant amount of weight, mostly from fat, but they also lost a meaningful amount of lean muscle at the same time.¹
Muscle plays a critical role in keeping metabolism active, supporting joints, and maintaining physical function. When muscle declines during rapid weight loss, people may feel weaker, experience more strain on their joints, and have a harder time keeping weight off once treatment changes or stops.
Independent experts reviewing multiple studies have shown that this pattern is not unique to tirzepatide. Reviews published in The Lancet Diabetes & Endocrinology show that lean muscle loss is common across all GLP-1 and GIP/GLP-1 medications, not an issue tied to one drug, dose, or manufacturer.²
The takeaway for plans and employers is clear. These medications are effective at lowering weight, but without a strategy to protect muscle, they introduce longer-term health and cost risks that do not appear in the first year of use.
Muscle loss is a predictable MSK cost multiplier
Muscle supports more than strength. It stabilizes joints, absorbs load, and enables efficient movement. The impact of members losing muscle takes a toll on healhcare outcomes (and on the downstream costs associated with subsequent MSK issues):
- Knees, hips, and the lower back absorb more stress
- Fatigue increases and activity levels decline
- Balance worsens, increasing fall and injury risk
MSK research shows that reduced muscle mass and physical deconditioning are associated with higher rates of pain, mobility limitation, and injury over time.³ ⁴ These changes rarely appear immediately as a single diagnosis. Instead, they tend to surface months later as increased use of musculoskeletal services, including physical therapy, imaging, and pain management.⁵ ⁶
For many employer health plans, this utilization pattern becomes visible well after early weight-loss success has been reported. By the time MSK claims rise, the connection to muscle loss during GLP-1 treatment is harder to trace, but the cost impact is real. This is why muscle loss functions as a multiplier. It quietly increases the likelihood and intensity of downstream MSK spend.
The strategic implication is clear. Tirzepatide coverage works better when it is paired with structured support that helps members preserve lean mass, maintain activity, and build habits that support healthier long-term outcomes after medication changes or stops.

What happens when tirzepatide is discontinued
Durability is another critical concern. In a follow-up study of people who stopped taking tirzepatide after losing weight, many regained a large portion of that weight within a year.⁷ Importantly, much of the regained weight was fat, not muscle.
This matters because losing muscle during treatment lowers the body’s ability to maintain weight once medication changes or stops. Members may end up with less muscle and more fat than before treatment, which increases functional risk and makes future weight management more difficult.
For plans, this dynamic often shows up as pressure to restart or extend therapy. Rather than tapering naturally, GLP-1 spend becomes prolonged, increasing per-member lifetime cost. Similar patterns have been observed with other medications in this class, which helps explain why lean mass loss during GLP-1 treatment is now a central concern for long-term sustainability.
The CFO view: how muscle loss quietly drives GLP-1 cost
From a financial perspective, the cost flow is straightforward.
Tirzepatide drives rapid weight loss. Rapid weight loss without muscle protection reduces metabolic efficiency and joint support. Over time, MSK complaints, fatigue, and injury risk increase. Claims shift toward physical therapy, imaging, and pain services. When treatment stops, weight regain increases re-prescription pressure. Per-member lifetime drug and MSK costs rise together.
This is why GLP-1 programs can look successful in year one and financially strained in years two and three, a dynamic already visible in analyses of GLP-1 employer healthcare costs and central to any sustainable GLP-1 cost savings strategy.
Movement protects weight loss investment
The encouraging news is that muscle loss is not inevitable. Research suggests that pairing GLP-1 and GIP/GLP-1 medications with resistance-based movement and adequate protein intake can help preserve lean mass.² ⁹ Members do not need high-intensity training or long gym sessions. Short, guided, strength-focused activity performed consistently can make a meaningful difference.
Medication changes the scale. Movement changes body composition. Only together do they deliver durable outcomes. Most members starting tirzepatide are inactive, managing prior pain, or unsure how to move safely. Simply telling people to exercise rarely leads to sustained behavior change. Without structure, safety, and accountability, muscle loss continues.
For employers and health plans, this is the controllable lever. Adding structured movement alongside medication coverage closes the gap that pharmacology alone cannot fill.
How Pulse supports tirzepatide users
Pulse, the cardiometabolic pillar of Sword's AI Care Platform, is designed to support people managing blood pressure, blood sugar, cholesterol, weight, and GLP-1 use through continuous lifestyle support. For people using tirzepatide, Pulse is built to address what medication alone does not: muscle preservation, strength-building support, nutrition guidance, and the day-to-day habits that help results last.
Pulse combines Phoenix, Sword Health’s AI Care Specialist, with guidance from a Health Specialist and connected devices that bring objective health data into each interaction. Members receive personalized support across movement, nutrition, and daily habits, with ongoing guidance that adapts over time to what is actually working for them.
How Pulse guides GLP-1 users to the right next step
1. Members describe their current goals and challenges: Pulse captures context around routines, symptoms, activity levels, and what kind of support feels realistic.
2. Guidance clarifies the right next step: Phoenix, Sword Health’s AI Care Specialist, helps members understand what to do next based on their daily reality and connected data.
3. Members receive support that fits their needs: Pulse can combine movement, nutrition guidance, and connected-device support, with a Health Specialist stepping in when nuance or clinical judgment matters.
4. Personalized support helps sustain measurable progress: The goal is not just early weight loss. It is helping members preserve strength, maintain function, and build habits that support long-term outcomes.
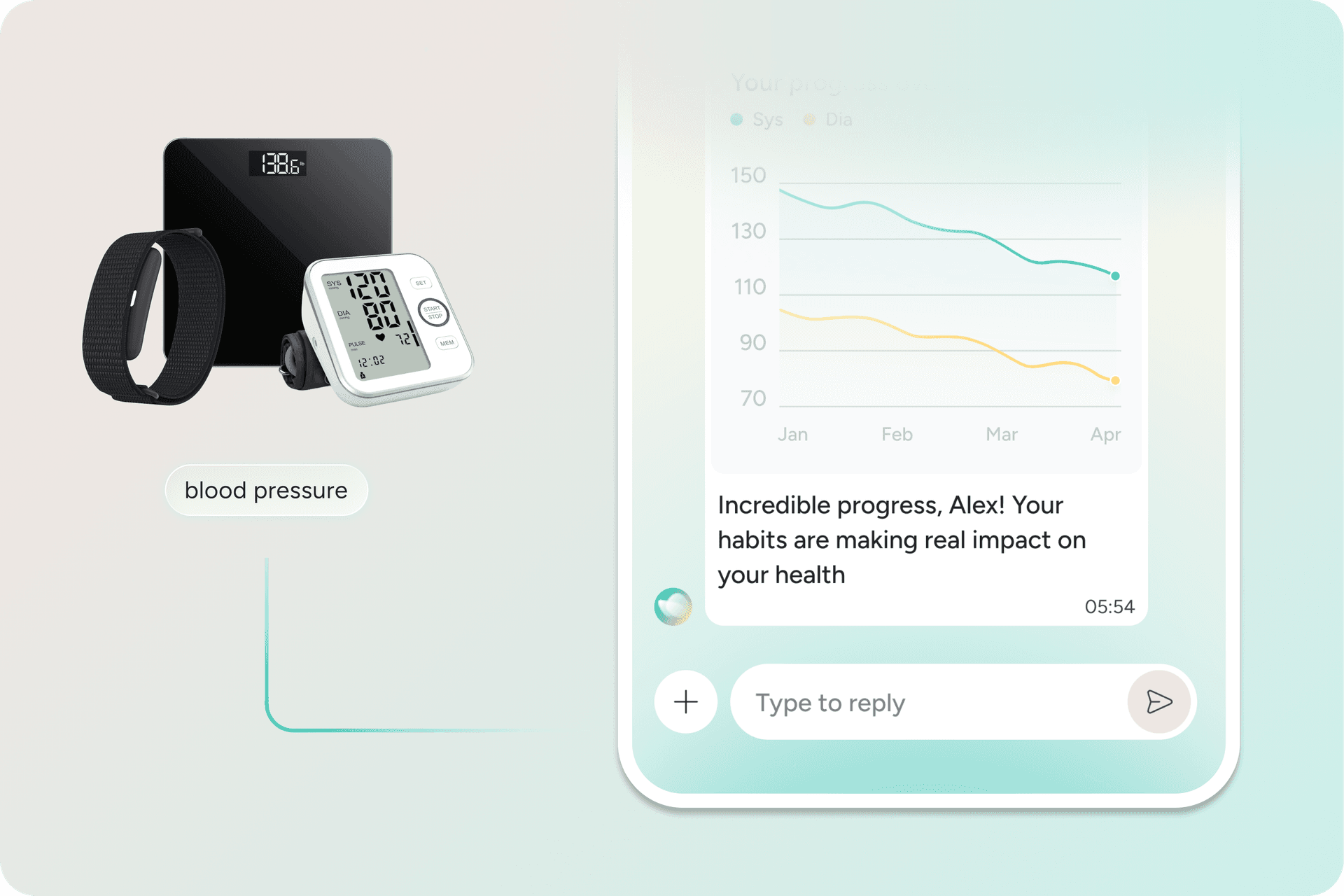
Build structured support around tirzepatide to protect GLP-1 spend
Pulse supports people using tirzepatide with continuous lifestyle support built around movement, nutrition guidance, and daily habits.
- 83% of members report feeling better or much better¹¹
- 51% of members with low physical activity at baseline reached the World Health Organization recommended activity threshold after 27 days of Pulse sessions¹²
Tirzepatide represents a major advance in weight management, and its impact on member engagement and short-term outcomes is undeniable. But weight loss alone is not the finish line. Without a strategy to protect muscle, rapid weight reduction can quietly introduce new risks that surface later as musculoskeletal claims, weight regain, and prolonged medication use.
By pairing tirzepatide coverage with Sword Pulse, health plan managers can help to:
- protect lean mass and function
- reduce downstream musculoskeletal risk
- improve the durability of weight-loss outcomes
- strengthen the long-term value of GLP-1 and GIP/GLP-1 investment
Pulse is designed to support people using tirzepatide with the continuous lifestyle support medication alone does not provide.
