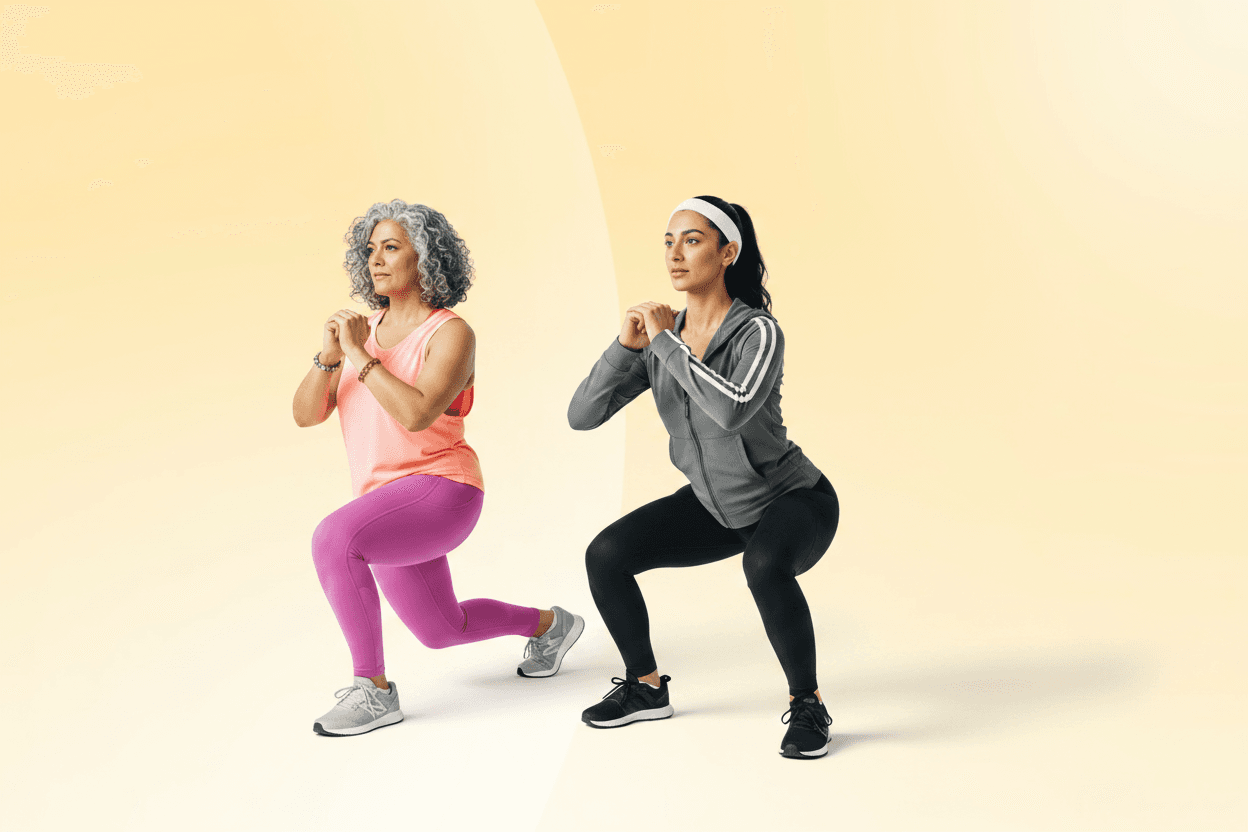Latest articles
Fresh healthcare insights

Stopping Mounjaro: how to keep the weight off
Mounjaro's dual mechanism produces deep metabolic gains. Here's what happens when you stop, and what the evidence says protects them.
May 8, 2026 • 7 min read

Stopping Wegovy: what happens and how to keep the weight off
Stopping Wegovy can lead to weight regain. Learn what happens to your body and how movement habits can help protect your results.
May 5, 2026 • 7 min read

Hip pain at night: why does it get worse when you sleep?
Hip pain that's worse at night is often related to inflammation, load, and your sleeping position. Learn why it happens and what you can do to help manage and prevent nighttime hip pain.
April 14, 2026 • 7 min read

Neck pain from desk work: why it happens and how to stop it
Desk-related neck pain is almost always about load, posture, and repetition. Not damage. Here's how to understand it and what actually helps.
April 14, 2026 • 6 min read

How to stop waking up with back pain every morning
If your back pain is most intense the moment you wake up, there's usually a reason. Learn what causes morning back pain and advice on how to manage the symptoms and stop the pain.
April 14, 2026 • 6 min read

Lower back pain when walking
Understand why walking triggers lower back pain and what you can do to manage symptoms, and when physical therapy is best to help you recover.
April 14, 2026 • 6 min read
Knee pain going up stairs: why it happens and what helps to recover
Stairs put more demand on your knee than flat ground. Learn why knee pain increases more often with stairs, and get practical strategies to help manage and reduce pain.
April 13, 2026 • 6 min read
For employers
Workplace health advice
How digital physical therapy improves employee retention
See how the right health benefits package can improve both employee retention and satisfaction.
October 24, 2025
GLP-1 employer healthcare costs: lower spend with better outcomes
Learn how GLP-1 programs can raise costs and why movement is the key to protecting outcomes and lowering employer spend.
October 23, 2025
How to evaluate and select the best digital MSK vendors
Find out how to evaluate the best MSK healthcare provider for your company when there are so many choices.
October 24, 2025
Reduce MSK costs with more effective digital MSK care plans
Find out why employers and benefits buyers must make reducing MSK costs a priority, and why digital MSK plans offer stronger ROI.
October 24, 2025
Expert guidance
From the experts: Ask a physical therapist

Ask a PT: Does walking really help with pain?
Megan Hill, Doctor of Physical Therapy, details a walking plan that anyone with pain can manage.
August 13, 2020

Ask a PT: What Is Causing My Shoulder Pain?
Discover the five most common causes of shoulder pain, how to tell them apart, and how to recover fast.
November 1, 2023

Ask a PT: when is the best time to do my exercises?
Megan Hill, Dr. of Physical Therapy, explores how and when to fit exercise into your busy schedule.
February 11, 2021
Healthcare contributors
Meet Sword's expert authors

Vijay Yanamadala
Chief Medical Officer at Sword Health

Megan Hill
Director, Clinical Specialists

Morgan Hollis
Head of Clinical Strategy, Sword Pulse

Liz Santo
Senior Clinical Program Manager, Sword Bloom ·

Jennesa Atherton
Head of Clinical Affairs, Sword Bloom

Fernando Correia
SVP Clinical & Regulatory Affairs at Sword Health